RESUMO
Introdução: A dor aguda e intensa faz parte do cotidiano dos pacientes que realizam cirurgia cardíaca, e para o controle da dor, pode-se dispor da analgesia controlada pelo paciente (PCA - Patient controlled analgesia). Objetivo: Comparar a analgesia utilizando PCA sem infusão contínua com PCA mais infusão contínua de morfina no pós-operatório de cirurgia cardíaca e avaliar a intensidade dolorosa, consumo analgésico, número de solicitações analgésicas, satisfação e efeitos colaterais. Métodos: Ensaio clínico randomizado em que foram estudados pacientes submetidos a cirurgias cardíacas, que utilizaram PCA com e sem infusão intravenosa de morfina. No pós-operatório, ao se extubar os pacientes, foi instalada PCA nas duas modalidades, conforme o sorteio. Intensidade dolorosa, consumo analgésico, número de solicitações analgésicas, satisfação e efeitos colaterais foram avaliados no momento da extubação e nas 6, 12, 18, 24 e 30 horas seguintes. Resultados: Foram avaliados 100 pacientes, sendo 50 no grupo (A) que recebeu PCA sem infusão contínua de morfina, e 50 no grupo (B) que utilizou PCA com infusão contínua de morfina. Pacientes do grupo (B) consumiram mais morfina, solicitaram menos vezes, e ficaram mais satisfeitos com a analgesia. Não se observaram diferenças significantes entre os grupos quanto à intensidade da dor e aos efeitos colaterais. Conclusões: O controle da dor foi eficiente e similar em ambos os grupos estudados. A mesma eficácia de analgesia e o menor consumo de morfina sugerem que PCA sem infusão contínua de morfina seja a melhor opção no controle da dor no pós-operatório de cirurgia cardíaca.
ABSTRACT
Introduction: Acute and severe pain is frequent in patients who undergo cardiothoracic surgery. Patient controlled analgesia (PCA) can be used to manage postoperative pain. Objective: To compare analgesia of morphine PCA alone (without continous infusion) with morphine PCA plus a continuous infusion on postoperative period after cardiac surgery and to evaluate pain scores, morphine consumption, number of demand, patient satisfaction and side effects. Methods: Randomized trial was conducted to assess patients who underwent cardiac surgery receiving either morphine PCA alone or morphine PCA plus continous infusion. In the post operative period, PCA was started at extubation in both regiments according to randomization. Pain intensity, morphine consumption, number of demand, satisfaction and side effects were assessed at zero, six, twelve, eighteen, twenty four and thirty hours after patients' extubation. Results: The study enrolled 100 patients. 50 patients received morphine PCA alone, (Group A) and 50 patients received morphine PCA plus a background infusion, (Group B). Group B patients had less demand, consumed more morphine and were more satisfied regarding analgesia. No statistical differences were shown between groups related to pain intensity, and side effects. Conclusions: Pain control was effective and similar in both groups. Morphine PCA alone seems to be better for postoperative pain manage in cardiac surgery, due to its less morphine expense with the same effectiveness.
INTRODUCTION
Postoperative pain is a complex process that results from afferent nociceptive nervous stimuli and central nervous system recognition caused by tissue surgery trauma. Management of acute pain has been a challenge for health professionals, several regiments and alternative methods have been described.
Patient controlled analgesia (PCA) is a well established mode of analgesia; despite its wide acceptance and use, controversies and questions remain. Using a remote infusion pump, patients are able to control the amount of opiates given either by intravenous or spinal routes improving their pain relief.
Some studies have favored PCA usage over regular administration of analgesics after abdominal, orthopedic and pediatric surgeries. PCA reduced level of pain with few side effects and promoted patient satisfaction [1-4].
There are also some controversies related to the route of PCA administration in the post operative period of cardiac surgery, although most agree spinal PCA is not often used probably because the risk of bleeding on the puncture site after heparin is given for cardiopulmonary bypass.
Cardiothoracic surgery is a very traumatic procedure. Sternotomy, ribs retraction, chest tubes, saphenectomy contribute to severe pain in the post operative period. Many treatment approaches such as non-steroidal anti-inflammatory drugs, opiates and local or regional anestesics have been used to decrease cardiac surgery patients' discomfort. PCA has been shown to be more effective than standard nurse-based pain therapy after cardiac surgery [5].
Two different regiments of intravenous morphine PCA have been clinically used. In one method, only intermittent morphine bolus is delivered for each request (morphine PCA alone). In the other, besides the intermittent bolus, a continuous morphine infusion is added (morphine PCA plus continuous infusion). Just a few studies have compared those modalities [6,7]. Although, It is not yet well established which form can offer better pain relief, with less side effects and drug consumption after cardiac surgery. Thus, this randomized controlled study was carried out with the aim to compare these two regiments after cardiac surgery.
METHODS
The study protocol was approved by the institutional ethical and research committee and patients were enrolled in the study after formal consent. The major eligibility criteria are listed in Table 1.
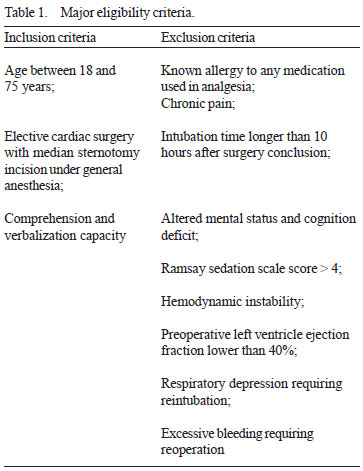

Data were prospectively collected on patients who were in the cardiac surgery postoperative period at the intensive care unit. All patients received dipyrone 1g intravenous every six hours. Infusion pump AMP Hospira® (Inc. Lake Forest, Illinois, U.S.A.) was installed after extubation. Subsequently, patients were randomly assigned by a computer generated sequence to receive either morphine PCA alone (Group A) or morphine PCA plus a continuous infusion (Group B). Patients were not aware of which analgesia mode they were on. Morphine 1mg was given for each request and continuous infusion was at a rate of 1 mg/h. Both groups had a 10 min lockout period and a safe higher limit of 40 mg in 4 hours. In order to assess analgesia, a research nurse who didn't know patients' group interviewed patients after extubation and every 6 hours until 30 hours. Patients were encouraged to answer a feedback form which described level of pain, localization, frequency, satisfaction and side effects.
Patients rated their level of pain using a verbal rating scale (VRS) from 0 to 10 (0 = no pain, 10 = the worst pain imaginable) and sedation was assessed using Ramsay's six-point scale (1 = anxious and agitated or restless or both; 2 = cooperative, oriented, tranquil; 3 = responds to commands only; 4= brisk response to a light glabellar tap or loud auditory stimulus; 5 = sluggish response to a light glabellar tap or loud auditory stimulus; 6 = no response to light glabellar tap or loud auditory stimulus). Assessment of satisfaction was done using a scale ranging from 0 to 10 (0 = no satisfaction, 1-4 = mild satisfaction, 5-7 = moderate satisfaction, 8-9 = satisfaction, 10 = extreme satisfaction) [8]. PCA demand and morphine consumption were collected from the data stored on the PCA infusion pump's memory. Any side effects observed during PCA use were registered.
Statistical analysis
Sample size was determined to detect a difference of 2 points in VRS between groups, SD of 3.5 with a power of the study of 80%. Therefore, 48 patients in each group would be necessary. Alpha-value of 0.05 was considered significant to apply the tests.
Student's t test was used for normally distributed variables and Mann-Whitney test when the values were not normally distributed. Comparisons of baseline clinical characteristics were performed with chi-square or Fisher's exact test for categorical data. For between-groups over time comparison, 2 way ANOVA was used. All analyses were done with the statistical package SPSS v. 10.0 (SPSS Inc., Chicago, IL, USA).
RESULTS
One hundred patients were enrolled in the study. It was observed more males 61 (61%) than females 39 (39%) and hypertension was the risk factor more prevalent present in 66 (66%). There were no significant differences between groups in baseline characteristics as shown in Table 2. Coronary artery bypass grafting (CABG) was the most performed procedure, 27 (54%) in Group A and 23 (46%) in Group B.
There were no significant differences in the position of chest tubes. In all moments evaluated, sternal incision and mediastinum drain insertion were the most common sites of pain related by the patients.
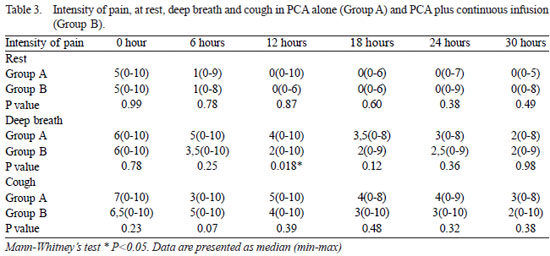
Either at rest or at deep breath or at cough mean VRS scores significantly lower after PCA was started and decreased progressively with time at each study period with no differences between groups, except at deep breath after 12 hours when Group B had better analgesia (Group B VRS 2 vs. Group A VRS 4, P=0.018). Table 3 describes patients' analgesia in all situations studied.
Although patients in Group A had to request more times (8.32 vs. 7.3 at 6hr, 6.38 vs. 3.98 at 12hr, 7.42 vs. 2.64 at 18hr, 5.62 vs. 2.3 at 24hr, 5.42 vs. 1.7 at 30 hr) P=0.27 as shown in Figure 1, Patients in Group B consumed significantly more morphine (7.2 mg vs. 12 mg at 6hr, 6.2 mg vs. 10.4 mg at 12hr, 6.4 mg vs. 9.3 mg at 18hr, 5.1mg vs. 8.1 mg at 24hr, 4.3 mg vs. 8.4 mg at 30hr) P<0.0001 as shown in Figure 2. Patients in both groups reported high rates of satisfaction with mean scores higher than 8.5. Patients in Group B tend to be more satisfied (8.5 vs. 8.5 at 6hr, 9 vs. 10 at 12hr, 9.5 vs. 10 at 18hr, 9 vs. 10 at 24hr, 9 vs. 10 at 36hr) and this was significant at 12, 24 and 30 hours. (P=0.04, <0.001, <0.001 respectively).
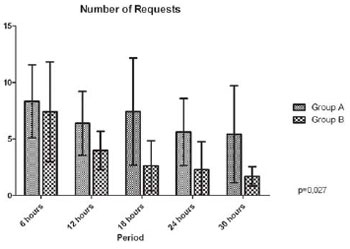
Fig. 1 - Comparison of morphine consumption between groups in all evaluated periods expressed in (mg) mean with 95% CI
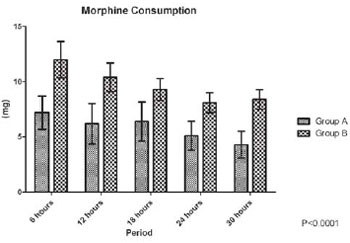
Fig. 2 - Groups comparison of mean number of requests in all evaluated periods with 95% CI
Nausea and vomiting was the most common adverse effects and there was no significant difference between groups related to those symptoms. Patients in Group B referred more pruritus although this difference was not significant. Respiratory depression was not observed in any patients. Table 4 shows the incidence of adverse effects in both groups.
DISCUSSION
Pain management is currently important and necessary as a basic right to all humans; moreover it is one measure of an institution's care quality of care. With new advances in the last decades and with better trained health care professionals, it has been possible to reduce acute post operative pain incidence, intensity and complications.
In order to better control post operative pain, it is necessary to quantify and to characterize pain correctly. Frequently patients feel moderate to severe pain due to under treatment.
Level of pain is difficult to access precisely; therefore VRS was used here because it's easy to comprehend. Therefore, efficacy of analgesia is evaluated by pain scores given by patients. Although VRS is not a perfect precise method of pain measure, it's an objective and reliable instrument of pain assess.
Some authors believe that the use of PCA plus a basal infusion may result in a better control of pain and decrease of additional requests [9,10]. Others state that basal infusion could increase medication consumption, side effects with no difference in pain relief as compared to PCA alone [1,6,11]. However, previous studies did not investigate these two different modalities of PCA in cardiac surgery patients. Our findings give a better view in this particular group of patients.
Comparing both groups concerning level of pain we found reduction at rest, deep breath and cough showing good benefit with PCA use. However, pain was not found at rest after 12 hours PCA was started but that was not observed at deep breath and cough. Moderate to severe pain predominates at deep breath just after extubation and became moderate to mild after PCA was started in both groups.
Even after 30 hours PCA was started, there were some patients who still reported intense pain. This result may be due to insufficient analgesia or other factors such as anxiety, personality, culture or any subjective nature that may interact in the pain process. Those were not studied in this research.
One study comparing intravenous morphine PCA versus PCA plus basal infusion with 60 patients who underwent coronary bypass have demonstrated that patients who received PCA plus basal infusion had pain scores significantly lower. However, another study involving morphine basal infusion enrolled 35 patients and was unable to show any significant difference in pain management when compared to PCA alone [12,13].
Mean morphine consumption in all study periods was higher in Group (B) as expected due to background infusion. Even though more morphine was used in Group (B), level of pain was the same in both groups.
On the other hand, despite patients in Group A received less opioid, they requested more often than patients in Group (B). Looking at each group independently, we found that Group (B) requested progressively less opioid over the evaluated period (P=0.0337), while this finding was not significant in Group (A) (P=0.0715), so continuous infusion might decrease earlier the need of demand.
Overall patients referred satisfaction with PCA even though they still had moderate to severe pain a few hours after PCA was started. However, patients in Group (B) was a significantly more satisfied at 24 and 30 hours.
According to previous reported data [14,15], we also observed that nausea and vomiting were the most common side effects. In this study, it occurred in the same way in both groups, respiratory depression which is the most serious adverse effect with morphine was not observed in any patient.
This study showed that both PCA modalities are very similar comparing level of pain, satisfaction, adverse effects. However, morphine consumption and possible side effects as reported by other studies [6,12,13,16] can help clinicians to choose the best alternative.
The present study didn't evaluate the costs in the different regimens; this issue could be interesting for further studies.
This study has some limitations, although we have used VRS, pain is subjective and there is an individual variability which is not measureable. Our results are based on how patients fell, assuming that an objective method makes possible a comparison. Other subjective variables, such as satisfaction, are difficult to measure by scales as well.
Although PCA is an automatic device, management of pain should always be individualized, and it should help heath care professionals to be closer offering the best care to their patients.
Pain management in the postoperative period of cardiac surgery was effective with PCA treatment and there was no significant difference with or without background infusion overall. However, there was an evident improvement in the level of pain mostly at cough and at deep breath after PCA was started.
In the beginning of PCA infusion, patients required opioid frequently but after same hours they required less and demand was lesser with background infusion.
As expected, PCA alone spent less morphine than with background infusion therefore this may have a cost issue. PCA was safe and there was no serious adverse effect with any modality. Satisfaction was more remarkable with background infusion.
Pain control was effective, safe and similar in both groups. However, we found that morphine PCA alone seems to be better for postoperative pain management in cardiac surgery, due to its less morphine expense with the same effectiveness when compared to morphine PCA plus continuous infusion.
REFERÊNCIAS
1. Doyle E, Robinson D, Morton NS. Comparison of patient-controlled analgesia with and without a background infusion after lower abdominal surgery in children. Br J Anaesth. 1993;71(5):670-3. [MedLine]
2. Choinière M, Rittenhouse BE, Perreault S, Chartrand D, Rousseau P, Smith B, et al. Efficacy and costs of patient-controlled analgesia versus regularly administered intramuscular opioid therapy. Anesthesiology. 1998;89(6):1377-88. [MedLine]
3. Vinik HR, Hammonds W, Len A. Patient-controlled analgesia (PCA) combined with continuous infusion. Anesth Task Analg. 1990;70:S418.
4. Egan KJ, Ready LB. Patient satisfaction with intravenous PCA or epidural morphine. Can J Anaesth. 1994;41(1):6-11. [MedLine]
5. Boldt J, Thaler E, Lehmann A, Papsdorf M, Isgro F. Pain management in cardiac surgery patients: comparison between standard therapy and patient-controlled analgesia regimen. J Cardiothorac Vasc Anesth. 1998;12(6):654-8. [MedLine]
6. Owen H, Szekely SM, Plummer JL, Cushnie JM, Mather LE. Variables of patient-controlled analgesia. 2. Concurrent infusion. Anaesthesia. 1989;44(1):11-3. [MedLine]
7. McKenzie R, Rudy T, Tantisiria B. Comparison of PCA alone and PCA with continuous infusion on pain relief and quality of sleep. Anesthesiology. 1990;73:A787. [MedLine]
8. Likert R. Rensis Likert on managing human assets. Bull Train. 1978;3(5):1-4. [MedLine]
9. Grass JA. Patient-controlled analgesia. Anesth Analg. 2005;101(5 Suppl):S44-61. [MedLine]
10. Romanek RM, Posso IP. Analgesia controlada pelo paciente no tratamento da dor pós-operatória. Rev Soc Bras Estudo da Dor. 2000; 2(2):15-25.
11. Parker RK, Holtmann B, White PF. Effects of a nighttime opioid infusion with PCA therapy on patient comfort and analgesic requirements after abdominal hysterectomy. Anesthesiology. 1992;76(3):362-7. [MedLine]
12. Guler T, Unlugenc H, Gundogan Z, Ozalevli M, Balcioglu O, Topcuoglu MS. A background infusion of morphine enhances patient-controlled analgesia after cardiac surgery. Can J Anaesth. 2004;51(7):718-22. [MedLine]
13. Dal D, Kanbak M, Caglar M, Aypar U. A background infusion of morphine does not enhance postoperative analgesia after cardiac surgery. Can J Anaesth. 2003;50(5):476-9. [MedLine]
14. Grass JA. Patient-controlled analgesia. Anesth Analg. 2005;101(5 Suppl):S44-61. [MedLine]
15. Viscusi ER, Reynolds L, Chung F, Atkinson LE, Khanna S. Patient-controlled transdermal fentanyl hydrochloride vs intravenous morphine pump for postoperative pain: a randomized controlled trial. Jama. 2004;291(11):1333-41. [MedLine]
16. Vinik HR, Hammonds W, Lett A, Kissin I. Patient Controlled Analgesia (PCA) combined continuous infusion. Anesth Analg. 1990;70(suppl):S418.
Article receive on quarta-feira, 15 de julho de 2009






 All scientific articles published at bjcvs.org are licensed under a Creative Commons license
All scientific articles published at bjcvs.org are licensed under a Creative Commons license