Priscila AikawaI; Angélica Rossi Sartori CintraII; Cleber Aparecido LeiteIII; Ricardo Henrique MarquesIV; Claudio Tafarel Mackmillan da SilvaV; Max dos Santos AfonsoV; Felipe da Silva PaulitschVI; Evandro Augusto OssVII
DOI: 10.5935/1678-9741.20130005
AMI: Acute myocardial infarction
CABG: Coronary artery bypass grafting
CAD: Coronary artery disease
CAT: Coronary arteriography
CHF: Chronic heart failure
CPB: Cardiopulmonary bypass
CRF: Chronic renal failure
DM: Diabetes mellitus
GA: Group of adult (patients < 65years-old)
GE: Group of elderly (patients > 65years-old)
ICU: Intensive care unit
MV: Mechanical ventilation
PVD: Peripheral vascular disease
SD: Standard deviation
SPSS: Statistical Package for the Social Science
INTRODUCTION
The growth of the elderly population, in absolute and relative numbers, is a worldwide phenomenon and is occurring at an unprecedented level. Currently, one in ten people aged 60 or older. In year 2050, it is estimated that the ratio will be one to five in the world, and one to three in developed countries. In Brazil, life expectancy has increased more than ten years (62.57 years to 73.17 years) and it is estimated that in 2050, the Brazilian population over 15% of people have 70 years or older [1].
Advanced age is a risk factor for development of coronary artery disease (CAD), diabetes mellitus, hypertension, dyslipidemia, smoking, obesity and family history of CAD. Elderly population has greater prevalence of CAD, and more inclinable to major coronary procedures as coronary artery bypass surgery (CABG). Additionally, cardiovascular disease is the major factor contributing to death, especially in elderly [2-4].
CABG is a safe procedure performed around the world with low rates of mortality and morbidity in the general population. The number of octogenarians undergoing CABG increased from 0.13%, in 1986, to 3.5%, in 2001, at the Heart Institute of the Clinical Hospital of the Faculty of Medicine, University of São Paulo, the last 16 years (1986-2001) [5]. Thus, recent studies demonstrate the concern of evaluating the outcomes of CABG in elderly patients and comparison with younger individuals to verify the risks to which the elderly are more vulnerable because they are considered high risk patients for this surgery [6,7].
Another important fact is that in the last decade, there have been many changes in surgical techniques, such as the advent of minimally invasive surgery, off-pump CABG, and new devices. Thus, the indication of CABG for elderly patients is increasing because it provides better survival and quality of life [8-12].
The aim of this study was to analyze the outcomes of CABG in patients aged 65 years or older compared with younger patients (<65 years) at a regional reference hospital in Southern Brazil.
METHODS
The project was approved by the Research Ethics Committee of the Hospital Associação de Caridade Santa Casa Rio Grande (RS, Brazil) under protocol number 001/2011.
This is a prospective study in which all patients who consecutively underwent CABG alone between 1st December 2010 to 31th July 2012 were analyzed at the Cardiology Hospital Doutor Pedro Bertoni of the Associação de Caridade Santa Casa Rio Grande (RS / Brazil). Patients undergoing CABG or associated with other cardiac surgery were excluded from the study. We included patients who needed surgery elective and urgent or emergency according to the criteria of the American Heart Association and the American College of Cardiology. Patients were divided into two groups, the group of elderly (GE) consisted of patients aged greater than 65 years and the adult group (GA) with patients under the age of 65. Data were collected daily directly from medical records and interviews with patients since its admission to discharge through a pre-structured form. All patients were elucidated on the research and signed an informed consent form.
The variables collected from the medical records and through interviews with patients were: sex, age, weight, height, race, comorbidities, prior CABG, prior coronary angiography, angioplasty surgery, sedentary lifestyle, smoking, alcohol consumption, number of grafts, time CPB, aortic clamping time, time of submission to mechanical ventilation (MV), length of stay in the Intensive Care Unit (ICU) and in the ward, postoperative complications and progression to hospital discharge or death.
The data were analyzed with the Statistical Package for Social Science (SPSS, version 13.0, Inc., Chicago, IL, USA). Continuous variables were expressed as means and standard deviations (SD), while categorical variables by proportions. Normality was checked using the Kolmogorov-Smirnov test. In the statistical analysis we used the Student t test to compare the means, and the chi-square or Fisher exact test to compare proportions. To determine which factors independently influence the development outcomes of the study was analyzed using multivariate logistic regression "stepwise forward". To verify the correlation between risk factors preoperative, intraoperative variables, postoperative variables and mortality was used the Spearman test. In all analyzes were considered significant when P <0.05.
RESULTS
During the study period, 253 consecutive patients submitted isolated on-pump CABG was assigned either Elderly Group (GE, n=103, 41%) or Adult Group (GA, n=150, 59%). The clinical and demographic characteristics of the patients are summarized in Table 1, which demonstrates a higher prevalence of males in both groups: GE = 61% and GA = 70%; no difference regarding gender, history of CAD in the family, hypertension, alcohol consumption, sedentary lifestyle, acute myocardial infarction (AMI), coronary angiography (CAT), previous angina pectoris, previous peripheral vascular disease (PVD), previous CABG, chronic renal failure (CRF) and failure chronic heart failure (CHF) and dyslipidemia. However, patients in the GA had a higher prevalence of diabetes mellitus (DM) (39.6% vs. 27%, P=0.043) and smoking (32.2% vs. 19.8%, P=0.042), whereas the GE patients had a higher prevalence of stroke prior (17% vs. 6.7%, P=0.013).
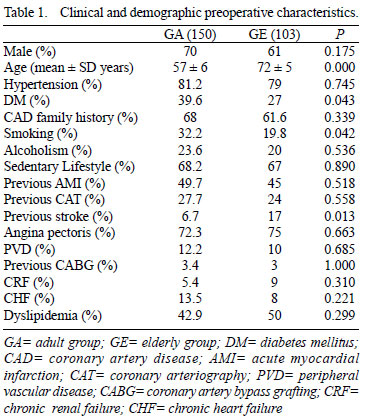
Table 2 shows the results of the surgery. There was no significant difference in mortality between the groups (P=0.165), but the rate of hospital morbidity was significantly higher in GE (30% vs. 14%, P=0.004).

Complications were divided into five categories: (1) hospitalization time in the two groups. In-ICU > 5 days was pulmonary complications: respiratory infection, (2) cardiac complications: arrhythmia, cardiac arrest, reinfarction, precordial pain and atrial fibrillation, (3) gastrointestinal complications: abdominal distension, (4) neurological complications: stroke, and (5) other complications: increased postoperative bleeding, mediastinitis, septic shock and sternal instability. There was no significant difference between the categories of complications comparing the groups.
Intraoperative data, MV and length of stay for both groups are shown in Table 3. There was no significant difference between groups in the time length of stay on MV <24 hours (P=0.096), MV between 24 and 48 hours (P=0.071) and MV> 48 hours (P=1.000); time of CPB (P=0.334) and aortic clamping (P=0.214), number of grafts (P=0.412), length of stay in ICU (P=0.140) and total time in hospital (P=0.144). However, the GE patients had more days hospitalized than patients in GA (P=0.036).
In Table 4, we analyzed the in-ICU and total in-greater in GE group (P = 0.010), but there is no difference in total in-hospital time between groups (P = 0.141).
After univariate analysis, the risk factors associated with hospital mortality were chronic renal failure, dyslipidemia, lin-ICU time > 5 days, in-ICU time, in-ward time, MV for more than 24 hours, CPB time, cardiac and respiratory complications. However, the age > 65 years was not a risk factor (Table 5).
After multivariate logistic regression analysis, the inward time (P=0.006), cardiac complications (P=0.011) and respiratory complications (P=0.026) were predictors of risk (P<0.05) for hospital mortality (Table 6).
In GE, we found that hospital mortality was positively correlated with length of stay in ICU > 5 days (P=0.008), MV > 48 hours (P<0.001), postoperative complications (P<0.001) and cardiac complications (P=0.004). Already in GA, hospital mortality showed positive correlation with DM (P=0.031), chronic renal failure (P=0.030), dyslipidemia (P=0.044), MV > 48 hours (P=0.029), postoperative complications (P<0.001) and respiratory complications (P<0.001).
DISCUSSION
This study in patients undergoing CABG alone suggests that patients aged > 65 years are subject to greater risk of postoperative complications than patients under 65, but there was no difference between the mortality rate between the groups.
Regarding to mortality rate, a study examining predictors of hospital mortality in patients undergoing CABG in acute myocardial analyzed that advanced age is a risk factor related to mortality [13]. Rocha et al. [14] also reported on a study conducted at the National Institute of Cardiology of Rio de Janeiro that the variables: age > 70 years, need for reoperation for revision of homeostasis, sepsis and respiratory complications postoperatively were associated with hospital mortality. As well, in another study in Santa Catarina/Brazil, the authors found the same relationship [15]. In our study, we found that age > 65 years was not a predictor of mortality, similar to other reported by Ng et al. [16] in a retrospective study with 1594 patients undergoing CABG alone, where no significant difference in hospital mortality between patients aged > 70 years (5.4%) compared to those with less than 70 years (3.8%). Even after 30 days of surgery, the mortality of patients aged > 70 years was 3.8% compared with 3.3% of patients aged <70 years (P<0.740).
The morbidity rate in hospital was higher in the GE compared to the GA. This data is in according to other study, which were also investigated the outcomes of CABG in elderly patients [14,17,18]. Pivatto et al. [19] observed that the morbidity rate was 34.4% in octogenarian patients undergoing CABG alone. We observed a morbidity rate of 30% in GE that was significantly higher compared to patients in the GA (14%). These data support the hypothesis that elderly patients have more postoperative complications.
In the GE, we founded that the prevalence of respiratory, cardiac, gastrointestinal, neurological, and other complications were higher compared to the GA, but there was no significant difference. Rocha et al. [14] observed that these complications were more developed for patients aged > 70 years, which had more respiratory complications (21.4% vs. 9.1%, P<0.001), mediastinitis (5.1% vs. 1.9%, P=0.013), stroke (3.9% vs. 1.3%, P=0.016), acute renal failure (7.8% vs. 1.3%, P<0.001), sepsis (3.9% vs. 1.9%, P=0.003), atrial fibrillation (15.6% vs. 9.8%, P=0.016) and 3rd degree atrioventricular block (3.5% vs. 1.2%, P=0.023) in the postoperative period compared to patients < 70 years-old.
In a retrospective study, Machado et al. [5] reported 10% mortality rate in octogenarian patients undergoing CABG, and observed the occurrence of cardiac arrhythmias (especially atrial fibrillation), cerebrovascular, and respiratory complications in the postoperative period. In our study, the cardiac complications were also major postoperative complications (12.6%). However, it was followed by respiratory complications (4.9%), and a lower incidence of neurological complications (1.9%).
Anderson et al. [20] observed predictors of mortality in patients undergoing cardiac surgery comparing septuagenarians and octogenarians, there was no significant difference in mortality rate between the groups. As observed in our study, preoperative variables did not increase the risk to death, but researchers have shown that cardiopulmonary bypass time > 75 minutes has 3.2 times (CI: 1.3 - 7.9) greater chance of to death than patients with cardiopulmonary bypass time < 75 minutes, and postoperative variables such as prolonged mechanical ventilation above 12 hours, length of stay in ICU, reoperation, inotropic support more than 48 hours, and the need for blood products are associated with increased mortality. In this study, we found that postoperative variables such as length of stay in hospital, and cardiac and respiratory postoperative complications are associated with higher mortality, suggesting that patients who had postoperative complications remained more time hospitalized, increasing the risk of mortality hospital.
Recently, in a retrospective study [14] with 655 patients undergoing CABG, the authors observed that length of stay in ICU > 3 days had positive correlation with death, but this study did not examine this relationship by age, and yes, total population sample. Our results show that length of stay > 5 days had positive correlation with death in GE, emphasizing the importance of studies that evaluate the outcomes of CABG in elderly patients.
Analyzing the most recent data in the literature, there is disagreement about what age, in elderly patients, the morbimortality appears to be significantly higher compared to adult patients. We found studies that described their groups of elderly with age > 65 years-old [12], > 70 years-old [13-17], > 75 years-old [6,21], > 80 years-old [22] and > 85 years-old [23]. Therefore we will suggest that more studies to be made in order to can to conclude in which age the risks factors of this surgery appear enlarged, whether preoperative, intraoperative or postoperative outcomes.
CONCLUSION
This study suggests that patients with 65 years old or more undergoing isolated on-pump coronary artery bypass surgery have a higher risk of postoperative complications in comparison with younger patients. The highest prevalence was heart complications, followed by respiratory complications; and lower prevalence of gastrointestinal and neurological complications.
REFERENCES
1. Brasil. Instituto Brasileiro de Geografia e Estatística (homepage). Brasília, DF. Ministério do Planejamento, Orçamento e Gestão; (tábuas completas de mortalidade 2008; comunicação social em 27.09.2008). Disponível em: http://www.ibge.gov.br Acesso em 01/10/2012.
2. Kurlansky P. Do octogenarians benefit from coronary artery bypass surgery: a question with a rapidly changing answer? Curr Opin Cardiol. 2012;27(6):611-9. [MedLine]
3. Rosamond W, Flegal K, Furie K, Go A, Greenlund K, Haase N, et al; American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics-2008 update: a report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation. 2008;117(4):e25-e146. [MedLine]
4. Veeranna V, Pradhan J, Niraj A, Fakhry H, Afonso L. Traditional cardiovascular risk factors and severity of angiographic coronary artery disease in the elderly. Prev Cardiol. 2010;13(3):135-40. [MedLine]
5. Machado LB, Chiaroni S, Vasconcelos Filho PO, Auler-Júnior JOC, Carmona MJC. Incidência de cirurgia cardíaca em octogenários: estudo retrospectivo. Rev Bras Anestesiol. 2003;53(5):646-53. [MedLine]
6. Rocha ASC, Pittella FJM, Lorenzo AR, Barzan V, Colafranceschi AS, Brito JOR, et al. A idade influencia os desfechos em pacientes com idade igual ou superior a 70 anos submetidos à cirurgia de revascularização miocárdica isolada. Rev Bras Cir Cardiovasc. 2012;27(1):45-5. View article
7. Al-Alao BS, Parissis H, McGovern E, Tolan M, Young VK. Propensity analysis of outcome in coronary artery bypass graft surgery patients >75 years old. Gen Thorac Cardiovasc Surg. 2012;60(4):217-24. [MedLine]
8. Eagle KA, Guyton RA, Davidoff R, Ewy GA, Fonger J, Gardner TJ, et al. ACC/AHA guidelines for coronary artery bypass graft surgery: executive summary and recommendations: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to revise the 1991 guidelines for coronary artery bypass graft surgery). Circulation. 1999;100(13):1464-80. [MedLine]
9. Task Force on Myocardial Revascularization of the European Society of Cardiology (ESC) and the European Association for Cardio-Thoracic Surgery (EACTS); European Association for Percutaneous Cardiovascular Interventions (EAPCI), Kolh P, Wijns W, Danchin N, Di Mario C, Falk V, Folliguet T. Guidelines on myocardial revascularization. Eur J Cardiothorac Surg. 2010;38(Suppl):S1-S52. [MedLine]
10. Braile DM, Leal JCF, Soares MJ, Godoi MF, Paiva O, Petrucci Júnior O, et al. Revasculação do miocárdio com cirurgia minimamente invasiva (MIDCAB): resultados em 46 pacientes. Rev Bras Cir Cardiovasc. 1998;13(3):194-7.
11. Shroyer AL, Grover FL, Hattler B, Collins JF, McDonald GO, Kozora E, et al; Veterans Affairs Randomized On/Off Bypass (ROOBY) Study Group. On-pump versus off-pump coronary-artery bypass surgery. N Engl J Med. 2009;361(19):1827-37. [MedLine]
12. Blacher C, Ribeiro JP. Cirurgia de revascularização miocárdica sem circulação extracorpórea: uma técnica em busca de evidências. Arq Bras Cardiol. 2003;80(6):656-62. [MedLine]
13. Mejía OAV, Lisboa LAF, Tiveron MG, Santiago JAD, Tineli RA, Dallan LAO, et al. Cirurgia de revascularização miocárdica na fase aguda do infarto: análise dos fatores preditores de mortalidade intra-hospitalar. Rev Bras Cir Cardiovasc. 2012;27(1):66-74. [MedLine] View article
14. Rocha ASC, Pittella FJM, Lorenzo AR, Barzan V, Colafranceschi AS, Brito JOR, et al. A idade influencia os desfechos em pacientes com idade igual ou superior a 70 anos submetidos à cirurgia de revascularização miocárdica isolada. Rev Bras Cir Cardiovasc. 2012;27(1):45-51.? [MedLine] View article
15. Oliveira EL, Westphal GA, Mastroeni MF. Características clínico-demográficas de pacientes submetidos à cirurgia de revascularização do miocárdio e sua relação com a mortalidade. Rev Bras Cir Cardiovasc. 2012;27(1):52-60. [MedLine] View article
16. Ng CY, Ramli MF, Awang Y. Coronary bypass surgery in patients aged 70 years and over: mortality, morbidity, length of stay and hospital cost. Asian CardiovascThorac Ann. 2004;12(3):218-23.
17. Johnson WM, Smith JM, Woods SE, Hendy MP, Hiratzha LF. Cardiac surgery in octogenarians: does age alone influence outcomes? Arch Surg. 2005;140(11):1089-93. [MedLine]
18. Alves Jr. L, Rodrigues AJ, Évora PRB, Basseto S, Scorzoni Filho A, Luciano PM, et al. Fatores de risco em septuagenários ou mais idosos submetidos à revascularização do miocárdio e ou operações valvares. Rev Bras Cir Cardiovasc. 2008;23(4):550-5. [MedLine] View article
19. Pivatto Jr F, Kalil RAK, Costa AR, Pereira EMC, Santos EZ, Valle FH, et al. Morbimortalidade em octogenários submetidos à cirurgia de revascularização miocárdica. Arq Bras Cardiol. 2012;95(1):41-6.
20. Anderson AJPG, Barros-Neto FXR, Costa MA, Dantas LD, Hueb AC, Prata MF. Preditores de mortalidade em pacientes acima de 70 anos na revascularização miocárdica ou troca valvar com circulação extracorpórea. Rev Bras Cir Cardiovasc. 2011;26(1):69-75. [MedLine] View article
21. MacDonald P, Stadnyk K, Cossett J, Klassen G, Johnstone D, Rockwood K. Outcomes of coronary artery bypass surgery in elderly people. Can J Cardiol. 1998;14(10):1215-22. [MedLine]
22. Peterson ED, Cowper PA, Jollis JG, Bebchuk JD, DeLong ER, Muhlbaier LH, et al. Outcomes of coronary artery bypass graft surgery in 24,461 patients aged 80 years or older. Circulation. 1995;92(9 Suppl):II85-91. [MedLine]
23. Guimarães IN, Moraes F, Segundo JP, Silva I, Andrade TG, Moraes CR. Fatores de risco para mortalidade em octogenários submetidos à cirurgia de revascularização miocárdica. Arq Bras Cardiol. 2011;96(2):94-98 [MedLine]
Supported by FUNADESP, Sao Paulo/Brazil, protocol number 5500255.
Article receive on Tuesday, October 30, 2012
 All scientific articles published at bjcvs.org are licensed under a Creative Commons license
All scientific articles published at bjcvs.org are licensed under a Creative Commons license