The authors describe the operative technique approach and its post-operative course used in an adult patient with coarctation of aorta, in which it was not possible to perform the traditional correction with an end-to-end anastomosis with graft interposition. During the surgery it was necessary to make an extra-anatomic bypass: ascending-descending aorta with an enlarged left posterior-lateral thoracotomy approach. The authors also make a short review of several possible approaches used for extra-anatomic bypass as well as its advantages and drawbacks.
Os autores relatam a técnica operatória empregada e a evolução clínica de um paciente adulto portador de coarctação de aorta (CoAo), no qual a correção tradicional com anastomose término-terminal com interposição de enxerto não foi possível. Durante o ato operatório, foi necessário mudar o planejamento e fazer um desvio extra-anatômico aorta ascendente-aorta descendente (Aoasc-Aodesc), via toracotomia póstero-lateral esquerda ampliada. Além disso, os autores fazem uma revisão sintética das várias abordagens possíveis usadas para os desvios extra-anatômicos e suas vantagens e desvantagens.
INTRODUCTION
Although the first surgery for repair of coarctation of the aorta (CoAo) was performed over 50 years ago, we often face complex cases turning traditional approaches impossible or very risky.
The traditional techniques for repair of coarctation of the aorta are resection of the narrowed area and end-toend anastomosis, with or without graft interposition; aorta surgically repaired by grafting a homograft "shaped like a Spanish roofing tile" in the narrowed area; and subclavian "flap" angioplasty. All these techniques are performed through left posterolateral thoracotomy.
The term complex CoAo refers to those cases in which associated heart lesions are present and repair surgery (aortic valve stenosis and bicuspid aortic valve disease; double dysfunction of aortic valve, coronary disease, etc.) is required, long narrowed route, hypoplastic aortic arch, and a very poor collateral circulation at the coarctation region. Regarding the associated lesions, it has been proposed a single approach via median sternotomy with an extra-anatomic ascending aorta-to-descending thoracic aorta bypass. This is achieved through a retrocardiac route in the posterior portion of the pericardium. In the event of hypoplastic long routes, extra-anatomic bypasses have been proposed as well. When the collateral circulation is poor, cardiopulmonary bypass can help to maintain medullar perfusion during aortic clamping time.
CASE REPORT
A.A.S.S. is a 28-year-old, male, asymptomatic patient who had a diagnosis of systemic arterial hypertension when he presented himself as a blood donor candidate. He was referred to the Serviço de Cardiologia da Irmandade de Misericórdia da Santa Casa de São Paulo, where a diagnosis of arterial hypertension secondary to CoAo was made. Echocardiogram showed left ventricular concentric hypertrophy, normal atrioventricular valves and semilunar cusps, and aortic segment stenosis in a 4.4 mm-postisthmic area.
He was referred to surgical treatment. A traditional repair surgery was planned with resection of the narrowed region and end-to-end anastomosis with graft interposition. After thoracotomy, a very close intraoperative analysis was performed and it was found an extensive stenosed segment at the isthmal and postisthmal area, presenting a poststenotic dilation making the access to aortic arch difficult. Resection of the later was required in order to allow aortic clamping in the region between left carotid artery and left subclavian artery.
The present anatomic situation was precluding the endto- end anastomosis even with tube interposition, besides the high bleeding risk. There was not another alternative except to perform an extra-anatomic bypass between ascending aorta-to-descending thoracic aorta. The anesthetist was asked to introduce the orotracheal cannula a little further in order to achieve right lung selective ventilation with left lung becoming collapsed. To get access to the superior potion of mediastinum and to the ascending aorta, it was necessary to section the 3rd and 4th ribs and to widen thoracotomy towards the sternum. Thus, after pericardial opening, an adequate ascending aorta exposition was accomplished.
The next step was to perform an end-to-side anastomosis connecting a 24 mm-Dacron Hemashield tube graft to the left anterolateral surface of the ascending aorta by partial aortic clamping using a polypropylene 3-0 thread.
After removing the air from the tube clamping was released, and it could be felt by digital palpation that there was a freely blood flow through the tube. A careful analysis of homeostasis and a thoracic drainage were performed afterwards. The sectioned ribs were fixed with stainless steel thread in the usual way.
The cardiothoracic surgeon is always liable to face unexpected situations, which become challenging and prompt changes in previous approach planned during surgical procedure. Constant dedication, hard study, and updating training are required to face these challenges.
The choice of the best technique to be used depends on the local and the extent of the stenosed area, the extent of the collateral circulation, and regarding coarctations the degree of adherence to the mediastinum.
Sometimes, surgical repair of aortic coarctation can become time-consuming and carry a great hemorrhage risk. The choice of an unconventional approach allows working out surgical repair and reducing the potential risk of a major hemorrhage. However, in order to choose the best approach, a very well-known knowledge of the stenosed region, isthmus involvement, collateral circulation, among others is necessary. Certainly, magnetic resonance image screening is very helpful in analyzing these aspects, but it is not always available, especially for patients receiving medical attention from the Single Health System (SUS).
If magnetic resonance imaging (MRI) screening provides the visualization of the left subclavian artery diameter, it is reduced; the surgeon must strongly consider another procedure rather than a bypass between left subclavian artery and the descending aorta. Moreover, MRI allows evaluating occasional approach difficulties of the precoarctation region through left 4th intercostals space thoracotomy, when the stenosed segment is extensive. In this case, the access to the aorta pre and postcoarctation can be easier through enlarged right thoracotomy, except when the left lung collapse is promoted through right lung selective intubation.
Cardiopulmonary bypass can be used: to repair coarctation of the aorta; to reduce spinal cord blood flow interruption risk, and in those cases in which local collateral circulation is considered poor. Furthemore, cardiopulmonary bypass helps to prevent marked hemodynamic changes in the extra-anatomic bypass technique when it is necessary to change heart's position to approach the retrocardiac descending thoracic aorta (median sternotomy approach).
In the literature, we found several approach methods for repair aortic coarctation through extra-anatomic bypass as follows:
1. Left posterolateral thoracotomy and Dracon tubular grafting anastomosis to the ascending aorta; passage of the graft anatomically parallel to the native aorta and grafting anastomosis to the descending thoracic aorta without approaching the stenosed area (Figure 1A).
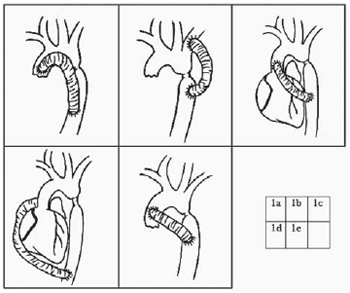
Fig. 1 - Plot of several approaches for management of aortic coarctation through extra-anatomic shunting
This technique was performed by Daebritz et al. [1] in children, when exist more tissue elasticity and the distance between the structure to be accessed is lower. However, it may be impossible or too risky to obtain an access to the ascending aorta via conventional left posterolateral thoracotomy (not enlarged) in adults.
2. Left thoracotomy and left subclavian artery bypass grafting to descending thoracic aorta [2] (Figure 1B).
This approach requires a prerequisite: in order to alleviate pre and postcoarctation pressure difference, the left subclavian artery diameter size must nearly parallel the descending thoracic aorta diameter size.
3. Left thoracotomy plus median sternotomy [3] (Figure 1C).
Left thoracotomy, grafting anastomosis to descending thoracic aorta, tunneling the graft below the hilum of left lung, and closure of thoracic cavity were performed. Patient is rotated 45°, median sternotomy and grafting anastomosis in ascending aorta is performed.
4. Enlarged right thoracotomy, grafting anastomosis in descending thoracic aorta, pericardial opening and ascending aorta exposure, and grafting anastomosis in the right anterolateral surface of ascending aorta is performed [4] (Figure 1D).
5. Median sternotomy (Figure 1E).
In 1980, Vijayanagar et al. [5] described an extra-anatomic ascending aorta-to-descending thoracic aorta bypass grafting anastomosis through median sternotomy with descending aorta exposure through posterior pericardial approach. This technique revealed itself attractive, especially in the cases of recoarctation, by avoiding direct dissection in the region of coarctation. In Brazil, Oliveira et al. [6] embodied significant experience with this approach. At first, grafting anastomosis in the descending aorta is performed and its exposure can be performed by slightly dislocating the heart forward. This can be facilitated with the patient in normothermic cardiopulmonary bypass. This technique is especially useful when a cardiac operation is necessary for associated lesions.
In the case report presented by the authors, the technique used was introduced by Daebritz et al. [1]. The difference was that the Dracon tubular graft rather than following a markedly curved route parallel to the native aorta followed a smaller route, passing next to the superior portion of the hilum of left lung (Figure 2). The patients of Daebritz et al. [1] were children in whom the distance between the structures and the tissue elasticity were lower, making the approach through thoracotomy, a routine procedure in surgical practice. Nevertheless, the authors believe that, in adults, it is impossible to approach the ascending aorta if the left thoracotomy is not enlarged with sections of costal arches and unless right lung selective intubation is performed.
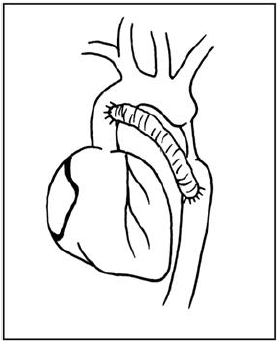
Fig. 2 - Plot of the surgery performed (left thoracotomy approach)
The authors wish to thank, Dr. Eduardo Gregório Chamlian, Thoracic Surgeon, Full Professor of Thoracic Surgery Discipline at IMSCSP for his help in preparing this study. Wendel R. Silva was responsible for the all plots, for which we are grateful.


 All scientific articles published at bjcvs.org are licensed under a Creative Commons license
All scientific articles published at bjcvs.org are licensed under a Creative Commons license