Considering that the world's population average age is increasing and the proportions of those over the age of 80, the fastest growing population worldwide, new approaches to health care and treatment will be necessary. Due to the development of new drugs and by means of transluminal coronary angioplasty or coronary artery bypass graft, many elderly patients had their lives prolonged and their quality of life improved. We carried out a bibliography review to search for evidence to support the best treatment choice according to the clinical manifestation of the patient.
Considerando que a média de idade da população mundial está aumentando e sendo a faixa etária superior a 80 anos a que cresce mais rapidamente em todo o mundo, novos enfoques de tratamentos e de cuidados se tornaram necessários para estas pessoas. Ante o desenvolvimento de novos produtos farmacológicos e de procedimentos por meio de angioplastia transluminal coronária ou cirurgia de revascularização miocárdica, muitos pacientes prolongaram sua vida e melhoraram a qualidade da mesma. Para indicar os procedimentos mais adequados, segundo as peculiaridades das manifestações clínicas, realizamos uma revisão bibliográfica com o objetivo de buscar evidências quanto ao benefício do tratamento cirúrgico ou da intervenção percutânea para este grupo de pacientes.
INTRODUCTION
The world's population average age is increasing and those over the age of 80 are the fastest growing population worldwide [1-3]. In 1998, according to United Nations data, approximately 66 million people were 80 years of age or older. This age group represents 1.1% of the world population. From 1970 to 1998, whereas the world population growth rate grew 60% the population 80 years of age or older rose 174% (from 26.7 to 66 millions). By the approaching year 2050, the proportion of those over the age of 80 is expected to increase by as much as sixfold (370 million people) [2].
In the United Kingdom, 1994, only 4% of population were 80 years of age or older. The United Kingdom population is projected to grow from 4% to 6% by 2020, corresponding to 3.6 million people [1]. In 1990, the number of people over the age of 80 in the United States was 6.9 million and it is expected a raise of more than 25 million by year 2050 [4]. In Brazil, according to the Brazilian Institute of Geography and Statistics or IBGE (Portuguese: Instituto Brasileiro de Geografia e Estatística) 1991/2000 data, 1.6% out of approximately 146.8 million inhabitants were 75 years of age or older [5]. Brazil is expected to have the 6th elderly world's population by the year 2020 [2].
The number of aged patients referred to coronary artery bypass grafting surgery (CABG) due to severe atherosclerotic disease has been increasing over recent years owing to an increase in expectation of life in general population [1,4,6,7]. Thus, the practitioners need to be prepared to attend structural, functional, and hemodynamic alterations related to aging in order to provide better strategies to promote healthy aging based on published evidence [2].
The elderly is expected to have a postoperative higher morbidity rate than younger people, despite the recent technological, pharmacological, and perioperative management breakthroughs that improve postoperative outcomes [4] as a result of the great number of patients with systemic diseases. Furthermore, aging promotes increasing structural heart changes, such as a greater deposition of fatty cells in the tissues and decreased vascular wall elasticity [2].
Ischemic heart disease (ischemic cardiomyopathy) is currently the leading cause of death in the elderly. Autopsy studies have shown a prevalence of coronary artery disease as high as 70% in this population. The prevalence of ischemic heart disease is markedly greater in elderly persons and approximately 20 to 30% of them are found to have a clinical presentation of ischemic disease [2].
Thus, to carry out the present study, we undertook a bibliographic review aiming at to seek for clinical evidence either regarding surgical treatment benefit or the percutaneous intervention for patients over the age of 75 presenting with ischemic heart disease.
An electronic search strategy was developed based on bibliographic review and scientific articles in order to identify studies and guidelines related to myocardial revascularization procedures in elderly patient with ischemic heart disease.
We searched the electronic database Medline for key articles published in the last 10 years, using as keywords the following: "bypass surgery", "percutaneous angioplasty", and "elderly". In addition, relevant studies carried out by Brazilian authors were also searched; especially those published by the Brazilian Journal of Cardiovascular Surgery (Revista Brasileira de Cirurgia Cardiovascular) and the Brazilian Archives of Cardiology (Arquivos Brasileiros de Cardiologia), both official scientific publications of the Brazilian Cardiology with the following keywords: "cirurgia de revascularização" (coronary artery bypass grafting surgery), "angioplastia" (angioplasty), and "pacientes octogenários" (octogenarian patients).
We also searched randomized clinical trials, meta-analyses, review articles, and consensus guidelines related to ischemic patients over 65 years old.
According to Figure 1 diagram, 330 articles were found to be potentially significant in Medline electronic database, of which 34 met all scientific rigour criteria.
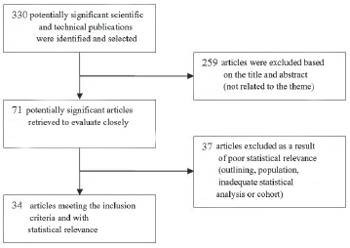
Fig 1 - Flow chart of the basedata scientific research strategy outcomes.
Patients with acute coronary syndrome (ACS) over the age of 80 are more likely to be hospitalized presenting with higher prevalence of heart failure, acute myocardial infarction, and renal failure. When undergoing angiography, these patients present with move severe coronary disease either with lesion involving three vessels or left coronary trunk lesion [8].
According to Halon et al. [8], in a study of 449 consecutive elderly patients to evaluate the importance of older age at admission and acute coronary syndrome outcome, the patients over 80 years old undergoing medical therapy have a worse survival than the younger ones (from 70 to 79 years old), however, in patients undergoing coronary artery bypass grafting the difference is small and not statistically significant among age groups. A 10-year increase in age is associated with a two times higher mortality rate in 24 months (17% for patients age ranged from 70 to 79 years and 33% for patients over 80 years old or older, p<0.0001) [8].
In accordance with GRACE (Global Registry of Acute Coronary Events), an observational record including 24,165 ACS patients in 102 hospitals in Europe, North America, South America, Australia, and New Zealand, hospital-mortality rates also increase with age as follows: 1.3% in patients < 45 years; 9.3% in patients age ranging from 75 to 84 years; and 18.4% in patients > or = 85 years (p=0.0001) [9].
A multicenter study sponsored by the American Heart Association has evaluated approximately 230,000 patients undergoing either CABG surgery or percutaneous coronary intervention (PCI) aiming to improve the understanding of these procedures regarding risks and outcomes. Between 1991 and 1999, the proportion of patients aged 75 years or older undergoing CABG increased as much as 10%. The in-hospital mortality risk associated with CABG per decade of life until 85 years of age, has increased 1% in patients undergoing PCI and 2% in patients undergoing CABG [10]. The mean mortality rate was 3% and 5.9% in patients undergoing PCI and CABG, respectively. The major in-hospital mortality risk predictors for PCI were emergencies, cardiogenic shock, or recent acute myocardial infarction. The best in-hospital mortality predictor for CABG was previous intervention [10,11].
The Alberta Provincial Project for Outcomes Assessment in Coronary Heart Disease (APPROACH), a clinical data collection and follow-up initiative capturing all patients undergoing cardiac catheterization in Alberta, Canada, was designed to compare meedical, surgical and percutaneous therapies in 21,573 patients stratified by age. In 15,392 patients > 70 years of age, the 4-year survival rates with CABG, PCI, and medical management were 95.0%, 93.8%, and 90.5%, respectively. In 5,198 patients 70 to 79 years of age, the 4-year survival rates were 87.3%, 83.9%, and 79.1%, respectively. Finally, in 983 patients e" 80 years of age, survival was 77.4% with CABG, 71.6% with PCI, and 60.3% with medical therapy. Reduced absolute risk in comparison to medical therapy for CABG (17.0%) and PCI (11.3%) were greater for patients < 80 years of age than for younger patients. The study stressed that elderly patients paradoxically have greater absolute risk reductions associated with surgical or percutaneous revascularization than do younger patients, suggesting that the benefits of aggressive revascularization therapies may extend to subsets of patients in older age groups [12].
Some studies identify the female gender, besides the age, as a predictor of increased incidence of postoperative complications. Basan et al. [13] compared the outcomes among elective revascularization surgical procedures in both women and men e" 80 years of age at the same time interval. Postoperative complications, including prolonged ventilation time, atrial fibrillation, sternal reclosure (sternal dehiscence), pneumonia, leg wound infection (post-saphenectomy surgical wound), and renal dysfunction have been found to be statistically significant in elderly women. There was no significant difference regarding mortality rate between male and female patients. Intensive care unit and hospital stays were also longer in female patients.
ACS was found to have higher incidence and poor prognosis without ST-segment elevation in elderly than in younger patients [2]. The early invasive approach strategy recommends running a routine cinecoronariography and myocardial revascularization with percutaneous or surgical procedure, depending on the circumstance [2].
Despite the following studies - TACTICS - TIMI 18 [14], FRISC II trial [15], RITA 3 [16], VINO [17], and TRUCS [18] - showing the benefits from early intervention strategy, this remains unclear as elderly patients present a rather increased complication risks regarding both catheterization and revascularization procedures, regardless the adopted procedure than the younger patients [14].
The Treat Angina with Aggrastat and Determine Cost of Therapy with an Invasive or Conservative Strategy-Thrombolysis in Myocardial Infarction (TACTICS-TIMI) 18 trial in 2,220 patients has shown increased in ACS elderly patients with non-ST-segment elevation acute MI undergoing early PCI compared to conservative management strategy. Among patients 65 years of age and older, the early invasive strategy compared with the conservative strategy yielded an absolute reduction of 4.8 percentage points (8.8% vs. 13.6%; p=0.018) and a relative reduction of 39% in death or MI at 6 months. Among patients older than 75 years of age, the early invasive strategy conferred an absolute reduction of 10.8 percentage points (10.8% vs. 21.6%; p=0.016) and a relative reduction of 56% in death or MI in the same time interval, despite increased hemorrhagic complications in this group regarding medical management strategy [14].
The Argentine Randomized Study: Coronary Angioplasty with Stenting Versus Coronary Bypass Surgery in Multi-Vessel Disease (ERACI II), a randomized, multicenter study comparing percutaneous coronary intervention (PCI) with stents over coronary artery bypass grafting (CABG) in 450 multi-vessel disease patients, has shown no significant difference at 5-year survival. However, patients undergoing PCI had increased incidence of repeat revascularization procedures in the same time interval [19].
In this way, the importance of PCI therapy in elderly patients is attributable, firstly, to the fact that elderly patients with unstable angina and non-ST-segment elevation myocardial infarction (MI) had significant increased adverse ischemic outcomes. Secondly, the early invasive management therapy reduces mortality or acute MI in elderly patients. Thirdly, the benefits from invasive management therapy are more significant and increase with age. Fourthly, by preventing coronary episodes, early invasive management reduces the health care costs. Fifthly and lastly, there is no increased incidence of stroke in elderly patients, despite the increased frequency in major bleeding complications [14].
The Bypass Angioplasty Revascularization Investigation (BARI), a randomized clinical trial, was designed to evaluate the survival in multivessel coronary artery disease patients over 65 years of age undergoing CABG or PCI management. After five years of follow-up, the survival rates were similar for both revascularization procedures [20]. However, after 7 years of follow-up, the survival rate in patients surgically treated was statistically superior (p=0.0425), especially in diabetic patients (p=0.0011) [21]. Eventually, at 10 years of follow-up, the authors have observed no significantly statistical difference regarding mortality or acute MI in non-diabetic patient groups [22]. The diabetic patients undergoing CABG had higher survival (57.8%) than the patients undergoing PCI (45.5%) in the same time interval (p=0.025) [22].
A Case-control cardiovascular disease study group from Northern New England compared the 8-year survival rate of approximately 15,000 coronary disease patients after both surgical and percutaneous management. Survival rates for patients with multivessel coronary disease were better after surgical revascularization than with percutaneous intervention (p<0.01), despite being older, having 3-vessel disease, and lower ejection fractions. The great advantage observed in patients treated with CABG was increased survival in 3-vessel disease patients, even considering women, diabetics, and the elderly and in the era of high stent utilization. There was no significantly statistical difference between both revascularization groups regarding 2-vessel disease patients [23].
Acute myocardial infarction is one of the leading current causes of death and 80% of the episodes affect patients over 65 years of age [2]. Age as a major mortality risk factor after acute MI was confirmed in a study by Batchelor et al. [24] comparing the clinical characteristics and in-hospital outcomes of 7,472 octogenarians with those of 102,236 patients < 80 years of age.
Recanalization of the coronary artery involved by means of fibrinolytic agents and percutaneous procedures has promoted a significant impact on acute MI, thus reducing its mortality to less than 10% [2].
The use of fibrinolytic agents to treat acute MI is conclusively beneficial in elderly patients, except for those over 75 years of age due to the increased incidence of hemorrhagic stroke [2].
Patients with acute myocardial infarction are increasingly being treated with percutaneous coronary intervention (PCI). In those patients with ST-elevation myocardial infarction (STEMI), primary angioplasty is used as an early reperfusion method, as rescue after fibrinolysis failure, or as part of an early invasive strategy. Similarly, an increase in the use of early invasive procedures has been observed to treat patients with non-ST-segment elevation myocardial infarction (MI). Abbott et all. [25], based on the National Heart, Lung and Blood Institute Dynamic Registry data, compared the clinical outcomes, including the treatment outcome, of consecutive patients undergoing PCI with ST-elevation myocardial infarction (STEMI) and non-STEMI (NSTEMI) at 1 year time interval at most. Patients with STEMI were younger, had fewer co-morbidities, and had less extensive coronary artery disease than did patients with NSTEMI. Angiographic success and periprocedural complications were similar in both groups. Coronary artery bypass grafting, stroke, bleeding and recurrent MI were similar but mortality was higher in patients with STEMI (p=0.004). Cardiogenic shock was associated with the greatest risk of in-hospital death (p=0.0001), but STEMI was also independently predictive of mortality. At 1 year, there was no need for repeat revascularization. However, patients with STEMI were more likely to undergo CABG in this time interval. Age, cardiogenic shock, renal disease, peripheral vascular disease, and cancer were predictive of death and MI. Multivessel disease and a larger number of >50% lesions were associated with the need for repeat revascularization [25].
Using the American College of Cardiology data, 8,828 patients over 80 years of age undergoing PCI at 145 participating centers were evaluated. The occurrence of acute MI was observed to be a strong predictor of mortality in this group. Overall in-hospital mortality was 1.35% for patients without myocardial infarction. Mortality rate for patients with acute MI between 24 h and one week prior to procedure was 4.39%. Mortality rate for patients with acute MI between 6 to 24 h prior to procedure was 9.87%, and for those patients who experienced acute MI 6 h prior to procedure, the mortality rate was 13.79% (p=0.0001) [26].
CHRONIC STABLE ANGINA
Chronic stable angina is defined by the unchanged symptoms due to ischemia for at least two months [2].
Chronic stable angina aims at the following: reduction of the symptoms, improvement of prognosis and quality of life, prevention of acute MI and sudden death. Regression or stabilization of the atherosclerotic plaque should be promoted; its complications should be prevented, especially thrombosis, and the myocardium should be protected with increased coronary blood flow. It is necessary to intervene in the risk factors to establish medical, surgical, or percutaneous therapy, according to the situation [2].
Percutaneous coronary intervention (PCI) is a widespread procedure for ischemic heart disease management performed, at first, using a balloon catheter and, recently, using stents [2]. In comparison to angioplasty alone, coronary artery stenting reduces the incidence of complications in the elderly [2], as well as restenosis rates. However, angiographic and clinical restenoses still occurs in a significant proportion of patients requiring repeat revascularizations and, consequently, they experience decreased quality of life and increased health care costs.
Many studies have sought convincing evidences to demonstrate that PCI is superior to drug therapy regarding both acute MI reduction and death in patients with ischemic heart disease. The Trial of Invasive versus Medical Therapy in the Elderly (TIME) was the first prospective, randomized clinical trial designed to compare an optimized medical strategy with an invasive strategy in patients e" 75 years of age. In a 4-year follow-up, mortality rate was similar for both types of treatment. Regarding other criteria (hospitalization, nonfatal cardiac events, and major events), invasive therapy was significantly better than medical therapy. When comparing myocardial revascularization performed by PCI versus CABG, it was verified that long-term mortality and reinfarction rates were similar for both therapies, but the need of repeat revascularization and the recurrence of symptoms have occurred more often in patients who underwent PCI [27.28].
The Clinical Outcomes Utilizing Revascularization and Aggressive Drug Evaluation (COURAGE) trial, involving 2,287 patients with approximately 60 years old at 50 U.S. and Canadian medical centers during a follow-up period of 2.5 to 7.0 years (median, 4.6), has proved that PCI does not reduce death, myocardial infarction, and stroke risk when associated to intensive medical therapy as an early strategy in patients with stable coronary artery disease [29].
The Arterial Revascularization Therapies Study (ARTS) was carried out during five years, at 67 centers involving 1,250 randomized patients to undergo either surgical therapy or PCI, has shown that both therapies (CABG/PCI) provide equally protection degree regarding death, acute MI, and stroke incidences in coronary disease patients with multivessel disease, except in diabetic patients. Among diabetic patients, those who underwent stent implantation had higher mortality rate (13.4%) compared to those who underwent CABG (8.3%). The incidence of repeat revascularization was significantly higher in the stent group (30.3%) than in the CABG group (8.8%; p < 0.001; RR, 3.46; 95% CI, 2.61 to 4.60) [30].
PERSPECTIVES FOR THE AGED PATIENT: OFF-PUMP CABG AND PHARMACOLOGICAL STENTS
It is further theorized which is the best surgical strategy for the aged patient: coronary artery bypass grafting (CABG) either with or without the use of cardiopulmonary bypass? A review of various clinical trials comparing the 2 surgical strategies, including several large retrospective analyses, meta-analyses, and the randomized trials that address different aspects of standard CABG and OPCAB have concluded that patients may achieve an outstanding benefit from off-pump CABG in the cases where the aorta is severely calcified and in which its manipulation and clamping can be associated to severe neurologic consequences, such as central embolic phenomena [31]. There has not been a definite answer yet regarding which strategy is the best one and in which patients should it be selected. Nowadays, however, the outcome with either strategy may rather depend on hospital structure, familiarity, comfort, and surgeon skill than the intrinsic benefit itself.
Regarding percutaneous coronary intervention, it is expected possible beneficial changes to avoid restenosis with drug-eluting stents advent [32], and the use of statins [33] and new antiplatelet drugs, especially in patients over 80 years old. Combined procedures, including pharmacological, percutaneous, and surgical therapies can become a beneficial option in selected cases, especially for aged and sicker patients. In relation to the PCI strategy, recent studies have brought out some new information that aid choosing the best management during the procedure. Lagerqvist et al. [34] have evaluated 6033 patients treated with drug-eluting stents, age ranging from 57 to 73 years (mean age, 65 years) and 13,738 patients treated with bare-metal stents, age ranging from 58 to 74 years (mean age, 66 years) in 2003 and 2004, using data from the Swedish Coronary Angiography and Angioplasty Registry (SCAAR). Drug-eluting stents were associated with an increased rate of death, as compared with bare-metal stents in a 3-year follow-up period. This trend appeared after 6 months, when the risk of death was 0.5 percentage point higher (adjusted relative risk for death in this group was 1.32; 95% CI, 1.11 to 1.57) and a composite of death or myocardial infarction was 0.5 to 1.0 percentage point higher per year (adjusted relative risk, 1.20; 95% confidence interval [CI], 1.05 to 1.37). From January 2002 through June 2005, Jensen et al. [35] evaluated 3,548 patients (5,422 lesions) who underwent implantation of drug-eluting stents (DES) and 8,847 patients (11,730 lesions) who underwent implantation of bare-metal stents (BMS). Patients' age ranged from 50 to 80 years. Postoperative antiplatelet regimen included acetylsalicylic acid (AAS), 75 mg to 150 mg per day, and clopidogrel with a loading dose of 300 mg, followed by a maintenance dose of 75 mg daily. The recommended treatment course with clopidogrel was 3- to 12-month courses until November 2002 and afterwards, 12-months courses. Over a 12-month follow-up, mortality was similar in both groups (p=0.22). At the same time interval, stent thrombosis (p=0.03) and acute MI risk (p=0.0001) occurred more frequently in patients undergoing implantation of drug-eluting stents compared to patients undergoing implantation of bare-metal stents. A meta-analysis of 14 trials [36] in which 4958 patients were 14 randomized to implantation of either bare-metal stents or drug-eluting stents and followed-up up to 59 months, has highlighted an increased late thrombosis rate with drug-eluting stent (0.6% versus 0.05%, p=0.02) when compared to the bare-metal-stent without increased adverse effects.
The Évaluation coût/efficacité du stent actif ou sirolimus chez les patients dabétiques et non diabétiques (EVASTENT), a multicenter study [37], has assessed the frequency and causes of stent thrombosis in diabetic and nondiabetic patients after implantation of sirolimus-eluting stents, in a cohort of 1,731 patients, age ranging from 50 to 80 years, of which 844 were diabetic. Patients were treated with aspirin + clopidogrel for at least 3 months and were followed for 465 days. Stent thrombosis rate was 1.8 times higher in diabetic than in nondiabetic patients (p=0.03), with diabetic patients with multiple-vessel disease experiencing the highest rate and nondiabetic single-vessel disease patients the lowest (p < 0.001) in the same time interval. In addition to the interruption of antithrombotic treatment, independent stent thrombosis predictors were previous stroke, renal failure, lower ejection fraction, calcified lesion, length stented, and insulin-dependent diabetes.
CONCLUSION
Based on the review of the literature, we have concluded the following:
1. There has been a gradual increase in the number of elderly patients undergoing myocardial revascularization either by percutaneous coronary intervention (PCI) or coronary artery bypass graft surgery (CABG);
2. Acute MI mortality rate is lower with early intervention therapy;
3. Aged ACS patients with non-ST-segment elevation have more benefits (lower mortality rate) with PCI and CABG therapies than with medical therapy;
4. It has been proved that for aged patients with stable angina, the benefit is not superior when percutaneous therapy is associated to surgical therapy as an early strategy;
5. The studies have demonstrated that the age factor is not sufficient to contraindicate any myocardial revascularization procedure techniques. Additionally, it has also been proved that surgical therapy poses a lower reduction in the need for reintervention when compared to percutaneous therapy;
6. Surgical therapy provides the better results. The more severe the case is, the lower is the risk reduction regarding the younger patients;
7. Finally, considering the recent world publications, it has to be evaluated the strictly use indication of either drug-eluting stents or bare-metal stents, once the literature, contrary to all expectations, has shown a greater risk of stent thrombosis associated with drug-eluting stents.

 All scientific articles published at bjcvs.org are licensed under a Creative Commons license
All scientific articles published at bjcvs.org are licensed under a Creative Commons license