The purpose of this paper is to present the late clinical results of mitral valve repair with the "Double Teflon" technique.
"Double Teflon" technique consists of a quadrangular resection of the posterior leaflet, annulus plication with "pledgetted" stitches over a Teflon patch, and leaflet suture. Between 1994 and 2003, 133 patients with degenerative mitral insufficiency due to ruptured or elongated chordae in the posterior leaflet underwent repair with this technique. The mean patient age was 60.4 years and 60.9% patients were male. According to clinical evaluation, 29.3% of the patients were in New York Heart Association functional class IV, 55.7% in class III and 15.0% in class II. Associated techniques of mitral valve repair were used in 15.2% of the patients; the most common was chordal shortening. Twenty six (19.5%) patients had associated procedures.
There was one (0.75%) operative death. In the late postoperative period, 95.5% of the surviving patients were in New York Heart Association functional class I. Linearized rates of thromboembolism, reoperation and death were 0.9%, 0.3% and 0.6% patient/year, respectively. The actuarial survival at 10 years was 94.7% ± 3.6%. Actuarial freedom from thromboembolism and reoperation were 97.3 ± 1.5% and 99.2 ±0.8%, respectively. There were no episodes of hemolysis or endocarditis.
Mitral valve repair with "Double Teflon" technique presents low morbimorbidity and good clinical late evolution.
O objetivo deste trabalho é apresentar os resultados clínicos tardios da plástica da valva mitral com a técnica do "Duplo Teflon".
A plástica de "Duplo Teflon" consiste em técnica de reparo mitral com ressecção quadrangular da cúspide posterior, anuloplastia segmentar com plicatura do anel com de fios com "pledgets" sobre uma tira de Teflon, e sutura borda a borda da cúspide. Entre abril de 1994 e dezembro de 2003, 133 pacientes com diagnóstico de insuficiência mitral degenerativa com alongamento ou rotura de cordas da cúspide posterior foram submetidos à plástica com esta técnica. A idade média foi de 60,4 anos e 60,9% eram do sexo feminino. Quanto à avaliação clínica no pré-operatório, 29,3% dos pacientes estavam em classe funcional IV, 55,7% em classe III e 15,0% em classe II. Técnicas associadas de plástica mitral foram utilizadas em 15,2% dos pacientes, sendo a mais comum o encurtamento de cordas. Vinte e seis (19,5%) pacientes foram submetidos a operações associadas.
Houve um (0,75%) óbito hospitalar. No período pós-operatório tardio, 95,5% dos sobreviventes estavam em classe funcional I. As taxas linearizadas de tromboembolismo, reoperação e óbito foram 0,9%, 0,3% e 0,6% pacientes/ano, respectivamente. A sobrevida atuarial em 10 anos foi de 94,1% ± 3,6%. As sobrevidas atuariais livre de tromboembolismo e reoperação foram de 97,3 ± 1,5% e 99,2 ± 0,8%, respectivamente. Não houve casos de endocardite ou hemólise.
A plástica da valva mitral com a técnica do "Duplo Teflon" apresenta baixa morbi-mortalidade e boa evolução clínica tardia.
INTRODUCTION
Mitral valve prolapse as a result of myxomatous degeneration evolves with a variety of clinical syndromes, which include mitral insufficiency in its most varying degrees. The most frequent mechanism of this insufficiency is the tendinous chordae elongation or rupture, especially in the posterior mitral leaflet. Currently, there exists a precise indication of mitral valve repair surgery. In many countries, the aforementioned mechanism is the most frequent cause of mitral insufficiency [1].
In a previous experience published in our service, this etiology corresponded to 25.9% of the patients undergoing mitral valve reconstruction [2]. Lower operative morbid-mortality, lower thromboembolism and endocarditis rates, better rates of survival, preservation of left ventricular function, reduced need of anticoagulation, and lower costs, all were accepted as advantages of mitral valve repair over replacement [3,6].
In patients with myxomatous degeneration with ruptured or elongated tendinous chordae of the posterior mitral leaflet, we have performed a quadrangular resection of the posterior mitral leaflet with similar results of those reported in the literature. In these patients, since April 1994, we have been using the 'double-Teflon technique' [7] without using prosthetic rings (Figure 1).

Fig. 1 - The 'double-Teflon technique
Mitral annulus undergoes periodical changes in size and shape throughout the cardiac cycle, contracting during systole. The reduction of mitral annular orifice area during systole is mainly due to contraction of posterior annulus [8]. The use of prosthetic mitral rings, especially the rigid rings, makes its normal contraction difficult. Studies have highlighted a better left ventricular systolic function in patients with flexible annuloplasty ring with a decreased left ventricular end-systolic diameter and volume [9]. In an experimental study in sheep performed by Dagun et al. [1], it was highlighted a significant difference in the mitral annular area after mitral valve repair with or without prosthetic ring.
The study aim was to present immediate and late results of mitral valve repair through the double-Teflon technique without prosthetic ring inpatients with mitral insufficiency secondary to myxomatous degeneration.
METHODS
Between April 1994 and December 2003, 133 patients diagnosed with mitral insufficiency with ruptured or elongated tendinous chords of the posterior mitral leaflet as a consequence of myxomatous degeneration underwent mitral valve repair with quadrangular resection by the double-Teflon technique at the Heart Institute (InCor), University of São Paulo Medical School, São Paulo, Brazil. The study was approved by the Clinic Hospital Ethics Committee of the University of São Paulo Medical School. Only patients with prolapse of posterior mitral leaflet alone were enrolled in the study. Patient age ranged from 25 to 89 years (mean age, 60.4 ± 11.9). Of the 133 patients, 80 (60.9%) were male and 53 (39.5%) were women. Regarding the postoperative clinical assessment, New York Heart Association (NYHA) functional class IV was present 29.3%, functional class III in 55.7%, and functional class II in 15.0% of the patients. Other cardiovascular diseases were present in 26 patients (19.5%) undergoing associated surgeries, such as myocardial revascularization in 18 (13.5%), replacement of aortic valve in 4 (3.0%), aortic comissurotomy in one (0.7%), and atrial septal defect repair in 3 (2.3%) of the patients.
Mitral valve injury intraoperative finding evidenced ruptured tendinous chordae in 69 (51.7%), elongated tendinous chordae in 41 (31%), and rupture associated with elongation of tendinous chordae in 23 (17.3%) of the patients. Significant calcification of the posterior mitral ring was observed in six (4.5%) of the patients. Regarding the posterior mitral leaflet segments affected, P1 was observed in 32 (24.2%), P2 in 78 (58.6%), and P3 in 23 (17.2%) of the patients.
Mitral repair associated techniques were used in 15% of the patients. Chordal shortening was the most common technique being performed in eight (6%) of the patients followed by mitral ring decalcification in six (4.5%), anterior leaflet wedge resection in five (3.7%), and posterior leaflet decalcification in one (0.7%).
Postoperative follow-up was carried out through hospital visits, phone interviews, or through mail questionnaire.
Data will be presented according to the reviewed guidelines of data and nomenclature presentation [11]. Actuarial survival and freedom of events were calculated by Kaplan-Meier method. The linearized rates of events are expressed in percentage by patient per year.
RESULTS
There was one in-hospital death (0.75%) due to stroke occurred on the postoperative day 6.
By the late postoperative period, 95.5% (124) of survivors were in NYHA functional class I, three (2.3%) in functional class II, two (1.5%) in functional class III, and one (0.7%) in functional class IV. The postoperative follow-up was 6684 months/patient.
There have been two late deaths (1.5%) due to acute myocardial infarction at a 15-month follow-up and one late death as a consequence of renal failure at a 6-month follow-up. Thromboembolism (minor events) has occurred in two (2.3%) patients as a result of two transient ischemic events within 40 days and 2 years postoperatively, respectively. One patient (0.7%) required reoperation after 72-month of follow-up due to rupture of another tendinous chord of posterior leaflet and underwent new mitral valve repair. The linearized rates for thromboembolism, reoperation, and late death were 0.9%, 0.3%, and 0.6%/patient-year, respectively. There were no episodes of hemolysis or endocarditis in this series.
Actuarial survival at 10 years was 94.1% ± 3.6% (Figure 2). The actuarial curves of freedom from thromboembolism (Figure 3) and freedom from reoperation (Figure 4) were 97.3% ± 1.5% and 99.2% ± 0.8%, respectively.

Fig. 2 - Actuarial survival
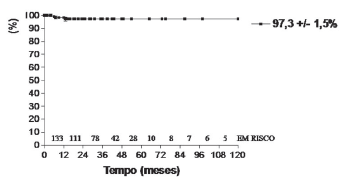
Fig. 3 - Freedom from thromboembolism - free actuarial curve

Fig. 4 - Freedom from reoperation - free actuarial curve
In patients with ruptured or elongated tendinous chordae of the posterior leaflet, we have performed a quadrangular resection of the posterior leaflet, posterior segmental annuloplasty by double-Teflon technique without prosthetic rings. Authors such as Carpentier et al. [12] and Gillinov et al. [13] advocate the use of prosthetic rings for quadrangular resection in order to stabilize the posterior mitral ring avoiding it to dilate again, thus augmenting the durability of mitral valve repair. In our clinical setting, Gregory et al. [14] and Carvalho et al. [15] also advocate the use of prosthetic rings in mitral valve repair with outstanding outcomes. However, as we demonstrated in this series, the survival freedom of reoperation at 10 years was 99.2% ± 0.8, which corroborates the durability of the mitral valve repair with this technique. Furthermore, there were no histological differences between the mitral ring of patients with myxomatous degeneration and that of normal patients [16].
Other authors, such as Alvarez et al. [17] demonstrated an estimate freedom from reoperation survival of 90.1% ± 4% at 10 years and 84.9% ± 11% at 15 years, using the quadrangular resection of posterior leaflet technique and annuloplasty without prosthetic ring, exactly as in our experiment. These authors have emphasized that the key stone for mitral valve repair with quadrangular resection success is the stability of the posterior mitral ring with a localized annuloplasty which withdraws the pressure on the reconstructed leaflet.
As a consequence of this procedure, the mitral valve posterior leaflet becomes a "plataform" against which the anterior leaflet opens and closes. The authors also emphasized that this technique does not affect the mobility of the anterior leaflet and that not using prosthetic ring shortens the duration of the operation, thus facilitating its reproducibility.
However, authors such as Eisnmann et al. [18] have also showed similar outcomes regarding quadrangular resection of the posterior leaflet without prosthetic rings with low immediate morbid-mortality and freedom from reoperation survival of 94% at 8 years. Barlow et al. [19] also recommend the resection of the posterior leaflet technique without the use of an annuloplasty ring, achieving satisfactory clinical and echocardiographic outcomes, what demonstrates the stability of the mitral valve repair without annuloplasty ring implantation.
Regarding in-hospital mortality (0.7%), our results are similar to other literature series [20,21]. David et al. [21], in a study involving 184 patients with mitral regurgitation due to degenerative disease, have stated that the mitral valve repair in mitral insufficiency due to myxomatous degeneration is feasible in the majority of the patients and it is associated with low morbid-mortality. The incidence of late complications was also low in this series presenting low linearized rate of events, similar to other literature series using quadrangular resection technique with or without ring annuloplasty [19,22]. In one series previously published [7], we have demonstrated good echocardiographic outcomes using this technique.
In a recent meta-analysis of 29 clinical trials comparing mitral valve repair to replacement, Shuhaiber and Anderson [23] found strong evidences favoring the mitral valve repair in degenerative etiology after 30 days and in late survival, which strengthens the use of mitral valve repair in this group of patient. Several groups advocate the indication of early surgery in these patients, even the asymptomatic ones, especially when there is ruptured or elongated tendinous chordae of posterior mitral leaflet, where the odds to undergo mitral valve repair is likely high, with fairly satisfactory published outcomes [24,25].
Based on favorable clinical outcomes regarding mitral valve repair in mitral insufficiency, especially insufficiency due to degenerative disease, with the double-Teflon technique, we considered this operative procedure of choice for patients with posterior mitral leaflet prolapse.
CONCLUSION
Mitral valve repair with double-Teflon technique without prosthetic ring employed in patients with mitral insufficiency secondary to myxomatous degenerative have presented a satisfactory rate survival and a good clinical outcome at 10-year follow-up.
REFERENCES
1. Galloway AC, Colvin SB, Baumann FG, Harty S, Spencer FC. Current concepts of mitral valve reconstruction for mitral insufficiency. Circulation. 1988;78(5 Pt 1):1087-98. [
MedLine]
2. Pomerantzeff PMA, Brandão CMA, Monteiro ACM, Nersessian AC, Zeratti AE, Stolf NAG, et al. Plástica da valva mitral: resultados tardios de doze anos de experiência e evolução das técnicas. Rev Bras Cir Cardiovasc. 1994;9(1):22-8.
3. Lee EM, Shapiro LM, Wells FC. Superiority of mitral valve repair in surgery for degenerative mitral regurgitation. Eur Heart J. 1997;18(4):655- 63. [
MedLine]
4. Enriquez-Sarano M, Schaff HV, Orszulak TA, Tajik AJ, Bailey KR, Frye RL. Valve repair improves the outcome of surgery for mitral regurgitation. A multivariate analysis. Circulation. 1995;91(4):1022-8. [
MedLine]
5. Westaby S. Preservation of left ventricular function in mitral valve surgery. Heart. 1996;75(4): 326-9. [
MedLine]
6. Barlow CW, Imber CJ, Sharples LD, Heriot AG, Wells FC, Large SR. Cost implications of mitral valve replacement versus repair in mitral regurgitation. Circulation. 1997;96(9 Suppl):II-90-3.
7. Pomerantzeff PM, Brandão CM, Souza LR, Vieira ML, Grimberg M, Ramires JA, et al. Posterior mitral leaflet repair with a simple segmental annulus support: the 'double-Teflon technique'. J Heart Valve Dis. 2002;11(2):160-4. [
MedLine]
8. Gatti G, Pugliese P. Preliminary experience in mitral valve repair using the Cosgrove-Edwards annuloplasty ring. Interact Cardiovasc Thorac Surg. 2003;2(3):256-61. [
MedLine]
9. David TE, Komeda M, Pollick C, Burns RJ. Mitral valve annuloplasty: the effect of the type on left ventricular function. Ann Thorac Surg. 1989;47(4):524-7.
10. Dagum P, Timek T, Green GR, Daughters GT, Liang D, Ingels NB Jr, et al. Three-dimensional geometric comparison of partial and complete flexible mitral annuloplasty rings. J Thorac Cardiovasc Surg. 2001;122(4):665-73. [
MedLine]
11. Edmunds LH Jr, Clark RE, Cohn LH, Grunkemeier GL, Miller DC, Weisel RD. Guidelines for reporting morbidity and mortality after cardiac valvular operations. Ad Hoc Liaison Committee for Standardizing Definitions of Prosthetic Heart Valve Morbidity of The American Association for Thoracic Surgery and The Society of Thoracic Surgeons. J Thorac Cardiovasc Surg. 1996;112(3):708-11. [
MedLine]
12. Carpentier A. Cardiac valve surgery: the "French correction". J Thorac Cardiovasc Surg. 1983;86(3):323-37. [
MedLine]
13. Gillinov AM, Cosgrove DM, Blackstone EH, Diaz R, Arnold JH, Lytle BW, et al. Durability of mitral valve repair for degenerative disease. J Thorac Cardiovasc Surg. 1998;116(5):734-43. [
MedLine]
14. Gregori F, Silva SS, Hayashi SS, Aquino W, Cordeiro C, Silva LR. Mitral valvuloplasty with a new prosthetic ring. Analysis of the first 105 cases. Eur J Cardiothorac Surg. 1994;8(4):168-72. [
MedLine]
15. Carvalho RG, Giublin PR, Lopes LR, Mulinari L, Loures DRR. Plástica da valva mitral com emprego do anel de Gregori-Braile: análise de 66 pacientes. Rev Bras Cir Cardiovasc. 1998,13(4):295-316.
16. Angelini A, Ho SY, Anderson RH, Davies MJ, Becker AE. Histological study of the atrioventricular junction in hearts with normal and prolapsed leaflets of the mitral valve. Br Heart J. 1988;59(6):712-6. [
MedLine]
17. Alvarez JM, Deal CW, Loveridge K, Brennan P, Eisenberg R, Ward M, et al. Repairing the degenerative mitral valve: ten- to fifteen- year follow-up. J Thorac Cardiovasc Surg. 1996;112(2):238-47. [
MedLine]
18. Eisenmann B, Charpentier A, Popescu S, Epailly E, Billaud P, Jirari A. Is a prosthetic ring required for mitral repair of mitral insufficiency due to posterior leaflet prolapse? Long-term results in 96 patients submitted to repair with no ring. Eur J Cardiothorac Surg. 1998;14(6):584-9. [
MedLine]
19. Barlow CW, Ali ZA, Lim E, Barlow JB, Wells FC. Modified technique for mitral repair without ring annuloplasty. Ann Thorac Surg. 2003;75(1):298-300. [
MedLine]
20. Braile DM, Ardito RV, Pinto GH, Santos JLV, Zaiantchick M, Souza DRS, et al. Plástica mitral. Rev Bras Cir Cardiovasc. 1990;5:86-98.
21. David TE, Armstrong S, Sun Z, Daniel L. Late results of mitral valve repair for mitral regurgitation due to degenerative disease. Ann Thorac Surg. 1993;56(1):7-12. [
MedLine]
22. Deloche A, Jebara VA, Relland JY, Chauvaud S, Fabiani JN, Perier P, et al. Valve repair with Carpentier techniques. The second decade. J Thorac Cardiovasc Surg. 1990;99(6):990- 1001. [
MedLine]
23. Shuhaiber J, Anderson RJ. Meta-analysis of clinical outcomes following surgical mitral valve repair or replacement. Eur J Cardiothorac Surg. 2007;31(2):267-75.
24. David TE, Ivanov J, Armstrong S, Rakowski H. Late outcomes of mitral valve repair for floppy valves: Implications for asymptomatic patients. J Thorac Cardiovasc Surg. 2003;125(5):1143-52. [
MedLine]
25. Smolens IA, Pagani FD, Deeb GM, Prager RL, Sonnad SS, Bolling SF. Prophylactic mitral reconstruction for mitral regurgitation. Ann Thorac Surg. 2001;72(4):1210-5.




 All scientific articles published at bjcvs.org are licensed under a Creative Commons license
All scientific articles published at bjcvs.org are licensed under a Creative Commons license