The aim of this study was to evaluate the applicability of the RACHS-1 (Risk Adjustment in Congenital Heart Surgery) as a predictor of surgical mortality in a pediatric population of a public hospital of the Northeast of Brazil.
From June 2001 through June 2004, 145 patients undergone surgical treatment of CHD in our institution of whom 62% were female, and the mean age was 5.1 years. The RACHS-1 was used to classify the surgical procedures into categories of risk 1 to 6, and logistic regression analysis was used to identify the risk factors related to surgical death.
Age, type of CHD, pulmonary flow, surgical procedure, pump time and cross clamp time were identified as a risk factor for postoperative mortality (p<0.001). There was a linear correlation between the categories of the RACHS-1 and the mortality rate; however, the observed mortality was greater than the predicted figures by that scoring system.
Although the RACHS-1 is easily applicable, it can not be applicable in our scenario because it takes into account only the surgical procedure as a categorized variable, not considering others factors presented in our scenario that could interfere in the final surgical result.
Avaliar a aplicabilidade do escore de risco ajustado para cirurgia de cardiopatias congênitas (RACHS-1) como preditor de mortalidade em uma população pediátrica de um hospital público da região Nordeste do Brasil.
No período de junho de 2001 a junho de 2004, 145 pacientes foram submetidos à correção de cardiopatia congênita em nossa instituição, dos quais 62% eram do sexo feminino, a idade média era 5,1 anos. Foi utilizado o escore de RACHS-1 para classificar os procedimentos cirúrgicos em categorias de risco de 1 a 6, e a análise de regressão logística para identificar os fatores de risco associados à mortalidade.
A idade, tipo de cardiopatia, fluxo pulmonar, tipo de cirurgia, tempo de circulação extracorpórea (CEC) e tempo de anóxia foram identificados como fatores de risco para mortalidade (p< 0,001). Houve correlação linear entre as categorias de risco do RACHS-1 e a taxa de mortalidade, entretanto, a mortalidade observada foi maior que a esperada por aquele sistema de escore.
A despeito da facilidade de aplicação do RACHS-1, ele não pode ser aplicado em nosso meio por não contemplar outras variáveis presentes em nossa realidade que podem interferir no resultado cirúrgico.
INTRODUCTION
Heart defects correspond to the most common congenital malformation affecting 8:1000 live births [1]. The early recognition of these defects is important as a result of its prognostic implication in face of the fast clinical deterioration and its high mortality rate. About 20-30% of the children with heart diseases die in the first month of life as a consequence of heart failure or hypoxia crises, and approximately 50% die until the end of the first year of life, when they do not receive adequate treatment [1,2].
In the last five years, great efforts have been made in the pursuit of quality assessment methods in thoracic surgery, especially for corrective or palliative procedures for congenital heart defects. Risk adjustment scores have been proposed to surgical procedures performed in children. Nevertheless, the wide diversity of heart defects is being suggested as a factor hampering consistent assessments [3]. In the world literature, there are more than 200 different diagnoses for congenital heart defects [2-4].
Given the large number of intervening variables in a surgical procedure, the search for a risk score is of vital concernment because it enables comparative assessment among distinctive services, allows inference as to the prognosis, and favors both surgical and patient/legal representative decision-making [3,4].
A special distinction in literature is given to the study by Jenkins et al. [3] who propose an easily applicable risk score, designated Risk Adjusted classification for Congenital Heart Surgery (RACHS-1). RACHS-1 was based on the categorization of several surgical procedures - palliative or corrective - which had similar in-hospital mortality. Therein, the diseases were assigned to six to one of six risk categories, according to the expected mortality rate predicted by each disease [3].
The aim of the present study is to evaluate whether RACHS-1 can be used as postoperative mortality predictor in congenital heart defects at a public university in the Northeast of Brazil.
METHODS
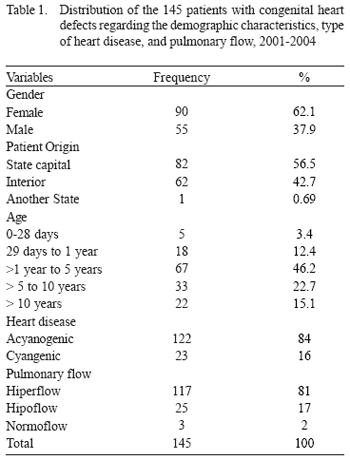
A prospective cohort was undertaken. The study population comprised all the patients under 18 years of age with congenital heart defects undergoing (corrective or palliative) thoracic surgery at our facility from June 2001 to June 2004. The exclusion criteria were patients undergoing surgical procedures which did not represent correction or palliation of congenital heart defect and patients with severe neurological lesion. The population initially identified comprised 160 patients. Of these, 15 patients were excluded; three of them had not undergone thoracic surgery and 12 were considered looses once their medical records could not be found. Patients' demographic characteristics are depicted in Table 1.
After the project approval by the Institutional Review Board, data collection from each patient's medical record was performed using an individual form in which the following data were surveyed:
A) Demographic variables: name, gender, age, patient origin, medical record number, weight, presence of other associated anomalies;
B) Surgical data: type of heart disease, type of surgery, pulmonary flow, CPB time, myocardial ischemia time, anatomical diagnosis;
C) RACHS-1 score (Risk Adjusted classification for Congenital Heart Surgery); and
D) Postoperative data: postoperative complications, deaths and cause of death.
Pulmonary hyperflow was defined by clinical criterion alone. Pulmonary hyperflow is the hemodynamic condition in which there is an increase of blood flow to the pulmonary artery.
The Risk Adjusted classification for Congenital Heart Surgery (RACHS-1) [3] was used in the present study to classify the population regarding surgical risk. Classification used is displayed in Panel 1.
Descriptive analyses were used to characterize the study population. Risk factors associated to postoperative mortality were further analyzed using the adjusted logistic regression model with a cutoff P value of 5% (pd"0.05).
There were no patients in RACHS-1 risk categories 5 and 6; all patients in RACHS-1 risk category 4 were excluded from the statistical analysis, once they represent only 1.3% of the study population.
A statistical program was used for all analysis of this study (STATA 8.0; Stata Corporation, College Station, TX).
RESULTS
During the observation period - June 2001 to June 2004 - 1035 surgical procedures were performed in our facility. Of the 1035 patients enrolled, 145 (14%) were included in our study.
Regarding the type of surgery, 93% of the patients underwent corrective surgery and as low as 7% underwent palliative surgery. The pulmonary-systemic anastomosis - the Blalock-Taussig anastomosis - was the most common palliative surgical procedure (n=8).
When the risk adjusted classification for congenital heart surgery (RACHS-1) was used, it was observed that the RACHS-1 category frequencies in our population were as follows: category 1: 53.7%, category 2: 34.4%, category 3: 15% and category 4: 1.3%. The latter were excluded from the statistical analysis. There were no patients in categories 5 and 6 (Table 2).
The accumulated in-hospital death (mortality rate) in this population was 17.2%. Deaths occurred in 60% of the male patients, 66% of which were over the age of one year. Cyanogenic heart diseases accounted for 66% of the deaths. Pulmonary hypoflow was present in 59% of the patients.
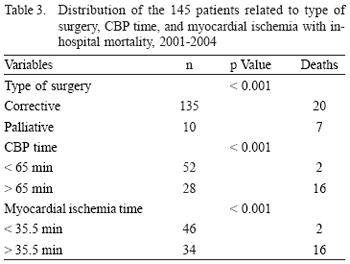
There has been a statistically significant correlation among the following variables: in-hospital death, type of correction surgery, CBP time, and myocardial ischemia (Table 3).
Among the causes of death, the most common was the low cardiac output syndrome, followed by pulmonary infection, which affected 48% and 11% of the patients, respectively. Other causes included ventricular arrhythmias and disseminated intravascular coagulation (DIC). The cause of death was not accurately identified in 7% of the patients.
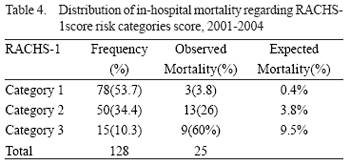
When the patients were stratified by risk category, the percentage of deaths was as follows: category 1: 3.8% and category 2: 26%, as shown in Table 4.
>
DISCUSSION
The present study reflects the experience of the first 2 years of a thoracic cardiac surgery at a public university service in the Northern region of Brazil, where abound associated difficulties to the diagnosis and management of these complex situations.
It is well-known in our setting that only 30% to 35% of the patients requiring thoracic surgery have access to palliative or corrective surgical therapy [5]. The Brazilian Cardiovascular Surgery Society report, 2004, demonstrates that there is a 65%-deficit in surgical interventions regarding congenital heart diseases in Brazil. The highest indices were found in the North and Northern regions (93.5% and 77.4%, respectively) [5]. Our hospital cardiology service is a hallmark for a population of nearly 6 million inhabitants [6]. According to the birth rate over the studied period, the population undergoing thoracic surgery at our surgical facility represented only 25% of the patients with congenital heart disease, when considered the incidence of congenital heart diseases for the number of live births in our State. Straightforwardly, these data reflect upon the difficulties such patients have to get medical care.
When the age group distribution was analyzed, it was noted that only 3.4% of the study population were in the neonatal period and only 12.9% were newborn infants (under the age of 1 year). In a study by Jenkins et al. [3] neonates were 19.1% and infants (under the age of 1 year) 31.6%. Other two authors presented outstanding percentages for each one of these age groups; Boethig et al. [7] found 18.7% for neonates and 38% for infants; Larsen et al. [8] reported 16% for neonates and 40% for infants.
Our findings reflect on how lately the patients are diagnosed and treated, which directly involves mortality rate as by chronic hypoxia, which leads to hypodevelopment and ponderal low weight gain in the Cyanogenic babies as for the chronic pulmonary hyperflow in the Cyanogenic babies, which leads to varying degrees of pulmonary hypertension.
The RACHS-1 score showed to be easily applicable because only the surgical procedure is an encoding variable; however, this easiness of application poses a series of questionings which are difficult to answer in our reality if we rely on in the surgical procedure alone, because the reality of our population is much different. In general, the cases are lately referred to surgery as it was demonstrated by the predominance of patients over the age of 1 year (46%).
Concerning mortality, our study shows a larger number of deaths in the group of cyanogenic heart diseases being in accordance with the literature which demonstrates to be the group of heart diseases with the highest mortality rates [5,9,10].
When we looked at death association and other variables, type of heart disease, pulmonary flow, type of surgical procedure, CBP time, and myocardial ischemia time were positively associated with, what was supported by international and national studies [11,13].
Regarding RACHS-1 risk score, it was observed that 100% of the study population could be classified in risk categories 1 to 4. This demonstrates how easy the score applicability is. In accordance with the original study by Jenkins et al. [3], it was observed a higher mortality rate in categories with higher risk scores.
The overall mortality rate of the present study is higher than in those using the same score [3,7,8] and certainly this reflect the learning curve for both teams, surgical and postoperative. This study shows the first two years of this service functioning, besides reflecting the reality of a facility - a low facility case volume - and it gets close to the mortality rate of other studies performed in populations similar to ours [9,14].
It is worth mentioning that the reference study to establish the score relied on a representative sample in a developed country, while our study population besides being limited was comprised of larger age groups surgeries of which were performed at the beginning of thoracic surgery experience in our public university facility located in the poorest demographic region of the country.
Furthermore, it is already established in the literature that other contributing factors for mortality after congenital heart disease surgeries are as follows: malnutrition, repeated respiratory infection (repeated upper airway infections, chronic respiratory infection), no previous clinical treatment, prematurity, and late diagnosis [13,15-20], which were also present in our study population, although they have not been analyzed because RACHS-1 score analysis does not include them, which turns to be a limitation of the method.
Clinical Significance
It is necessary to implement the risk models in congenital heart disease surgeries adjusted to the reality features of Brazil.
CONCLUSION
Despite being easily applicable, RACHS-1 score cannot be used in our setting, because it does not include other variables present in our reality, which can interfere with the surgical outcome.
REFERENCES
1. Silva CMC, Gomes LFG. Reconhecimento clínico das cardiopatias congênitas. Rev Soc Cardiol Estado de São Paulo. 2002;12(5). Disponível em: http://www.socesp.org.br
2. Kirklin JW, Kouchoukos NT. Kirklin/Barrat-Boyes Cardiac Surgery: morphology, diagnostic criteria, natural history, techniques, results and indications. Pennsylvania:Elsevier; 2003.
3. Jenkins KJ, Gauvreau K, Newburger JW, Spray TL, Moller JH, Iezzoni LI. Consensus-based method for risk adjustment for surgery for congenital heart disease. J Thorac Cardiovasc Surg. 2002;123(1):110-8. [
MedLine]
4. Lacour-Gayet F, Clarke D, Jacobs J, Comas J, Daebritz S, Daenen W, et al. The Aristotle score: a complexity-adjusted method to evaluate surgical results. Eur J Cardiothorac Surg. 2004;25(6):911-24. [
MedLine]
5. Pinto Jr VC, Daher CV, Sallum FS, Jatene MB, Croti UA. Situação das cirurgias cardíacas congênitas no Brasil. Rev Bras Cir Cardiovasc. 2004;19(2):III-VI.
6. DATASUS- disponível em URL: www.datasus.gov.br
7. Larsen SH, Pedersen J, Jacobsen J, Johnsen SP, Hansen OK, Hjortdal V. The RACHS-1 risk categories reflect mortality and length of stay in a Danish population of children operated for congenital heart disease. Eur J Cardiothorac Surg. 2005;28(6):877-81. [
MedLine]
8. Boethig D, Jenkins KJ, Hecker H, Thies WR, Breymann T. The RACHS-1 risk categories reflect mortality and length of hospital stay in a large German pediatric cardiac surgery population. Eur J Cardiothorac Surg. 2004;26(1):12-7. [
MedLine]
9. Castillo VR, Jaramillo GA, Andrade OH, Montro A, Salazar L, Sanbria J, et al. Mortalidad quirúrgica de la corrección de cardiopatias congênitas en la Fundación Cardiovascular de Colômbia: 2000-2005. Rev Col Cardiol. 2007;13(2):132-5.
10. Kang N, Cole T, Tsang V. Risk stratification in paediatric openheart surgery. Eur J Cardiothorac Surg. 2004;26(1):3-11. [
MedLine]
11. Aylin P, Bottle A, Jarman B, Elliott P. Paediatric cardiac surgical mortality in England after Bristol: descriptive analysis of hospital episode statistics 1991-2002. BMJ. 2004;329(7470):825. [
MedLine]
12. Chang RK, Chen AY, Klitzner TS. Female sex as a risk factor for in-hospital mortality among children undergoing cardiac surgery. Circulation. 2002;106(12):1514-22. [
MedLine]
13. Reddy VM, Hanley FL. Cardiac surgery in infants with very low birth weight. Semin Pediatr Surg. 2000;9(2):91-5. [
MedLine]
14. Mattos SS, Neves JR, Costa MC, Hatem TP, Luna CF. An index for evaluating results in paediatric cardiac intensive care. Cardiol Young. 2006;16(4):369-77. [
MedLine]
15. Spiegelhalter DJ. Mortality and volume of cases in paediatric cardiac surgery: retrospective study based on routinely collected data. BMJ. 2002;324(7332):261-3. [
MedLine]
16. Allen SW, Gauvreau K, Bloom BT, Jenkins KJ. Evidencedbased referral results in significantly reduced mortality after congenital heart surgery. Pediatrics. 2003;112(1 Pt 1):24-8. [
MedLine]
17. Welsby IJ, Bennett-Guerrero E, Atwell D, White WD, Newman MF, Smith PK, et al. The association of complication type with mortality and prolonged stay after cardiac surgery with cardiopulmonary bypass. Anesth Analg. 2002;94(5):1072-8. [
MedLine]
18. Hewitson J, Brink J, Zilla P. The challenge of pediatric cardiac services in the developing world. Semin Thorac Cardiovasc Surg. 2002;14(4):340-5. [
MedLine]
19. Jenkins KJ, Newburger JW, Lock JE, Davis RB, Coffman GA, Iezzoni LI. In-hospital mortality for surgical repair of congenital heart defects: preliminary observations of variation by hospital caseload. Pediatrics. 1995;95(3):323-30. [
MedLine]
20. Calderón-Colmenero J, Flores A, Ramírez S, Patiño-Bahena E, Zabal C, García-Montes JA, et al. Surgical treatment results of congenital heart defects in children with Down's syndrome. Arch Card Mex. 2004;74(1):39-44.
Article receive on Sunday, August 12, 2007


 >
> All scientific articles published at bjcvs.org are licensed under a Creative Commons license
All scientific articles published at bjcvs.org are licensed under a Creative Commons license